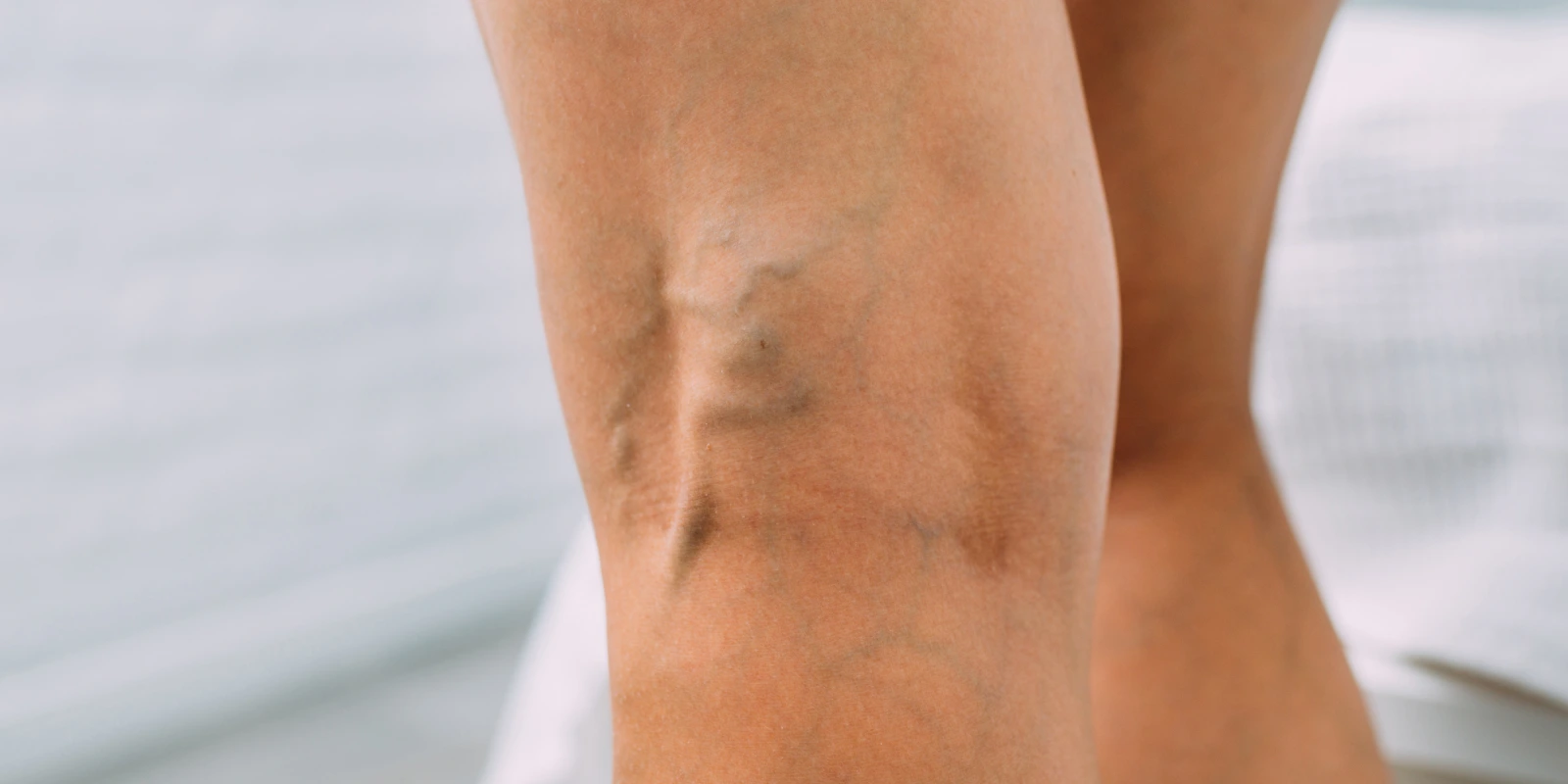
“This is just cosmetic.”
That was the reassurance one of my patients had received repeatedly over the years. She worked long hours on her feet and described aching, heaviness, and visible veins that made her both uncomfortable and frustrated. For her, the issue was not only appearance; her symptoms were interfering with daily life.
Listening to her, it became clear that her concern was more than skin-deep. The encounter reminded me that what often seems like a minor complaint can, in fact, be the first signal of a larger health problem.
More Than Cosmetic
Varicose veins are frequently minimized, yet they represent one of the most visible manifestations of chronic venous insufficiency (CVI). In CVI, dysfunctional venous valves allow blood to pool, leading to venous hypertension and progressive tissue changes.
The Society for Vascular Surgery and American Venous Forum guidelines provide a comprehensive framework for evaluating and managing CVI, emphasizing early recognition, duplex ultrasound assessment, and the role of compression and lifestyle measures as first-line therapy.
Clinically, it helps to remember a few key points:
- Symptoms matter: Heaviness, aching, swelling, or night cramps should raise suspicion for venous disease.
- Skin tells the story: Hyperpigmentation, stasis dermatitis, or induration are warning signs of progression.
- Complications are significant: Untreated disease can result in venous ulcers, recurrent cellulitis, and even thrombotic events, as highlighted in AAFP guidelines on varicose veins.
When varicose veins are dismissed as cosmetic, we miss the opportunity to intervene early and prevent morbidity.
The Role of Primary Care
Most patients do not walk into a vascular clinic as their first step. They present to their family physician or internist, which means primary care is often the front line for venous disease.
A focused history and a brief inspection of the legs can uncover early disease. From there, practical measures make a meaningful difference:
- Counseling on weight management, mobility, and leg elevation
- Initiating compression therapy to reduce symptoms (ACC nonsurgical management of CVI)
- Screening for comorbidities such as diabetes, hypertension, and dyslipidemia
- Referring to vascular specialists when quality of life is impaired or advanced skin changes are present
Even brief interventions signal to patients that their concerns are valid and worth addressing.
A Window Into Prevention
For me, working with venous disease has underscored how often it overlaps with cardiometabolic risk factors. Obesity, sedentary lifestyle, and metabolic syndrome are common companions.
One patient who sought care for “ugly veins” was also found to have uncontrolled hypertension and newly diagnosed type 2 diabetes. Her varicose veins became the entry point into a broader preventive conversation.
Encounters like these reinforce the importance of reframing venous disease. It is not merely a localized cosmetic problem but a potential marker of systemic health.
What These Patients Have Taught Me
Patients with venous disease have left me with several enduring lessons:
- Respect the complaint: What appears minor may weigh heavily on patients and deserve careful attention.
- Look deeper: Visible venous changes can be the surface marker of underlying systemic disease.
- Prevention is opportunistic: Sometimes the opening to discuss cardiovascular risk begins with a conversation about tired, heavy legs.
These experiences remind me that the clinical value of an encounter often extends far beyond the presenting complaint.
Conclusion
Varicose veins are not trivial. They are a visible sign of venous dysfunction and an opportunity for early recognition, education, and preventive care.
For those of us in primary care, the patient who lifts a pant leg to show “just cosmetic veins” is not only asking us to comment on appearance. They may be giving us the first chance to intervene for their venous health and their overall vascular health.
Because sometimes the smallest concerns, if taken seriously, can lead to the greatest preventive impact.
When have you uncovered a broader health issue that began with what seemed like a minor complaint? Share in the comments.
Shafi S. Rana, MD, MBA, is a board-certified family medicine physician in New York. His clinical work spans obesity and vascular medicine, with a focus on cardiometabolic disease and longitudinal care. He integrates medical expertise with experience in finance, physician leadership, and health system operations to strengthen patient outcomes and organizational performance. His interests include the thoughtful integration of AI and emerging technologies to improve access, quality, and long-term value in health care. He is a 2025–2026 Doximity Op-Med Fellow.
Image by ilikeyellow / Shutterstock