I was invited to present an update on “What is New in Women and Heart Disease?” at the American Heart Association Scientific Sessions in Philadelphia from November 9 to 12, 2023. As the medical director of the Rush Heart Center for Women for 20 years, I have learned a lot from taking care of hundreds of women with or at risk for heart disease. The following is a summary of the current state of the art on how to help women with ischemic heart disease and heart failure. I also discussed maternal mortality and the link between heart disease and breast cancer.
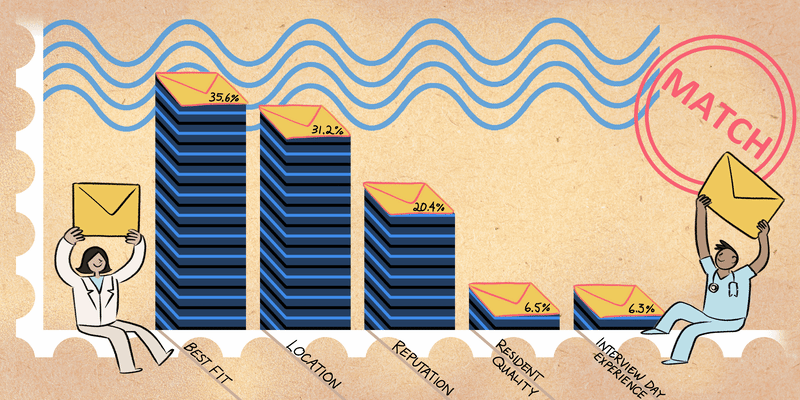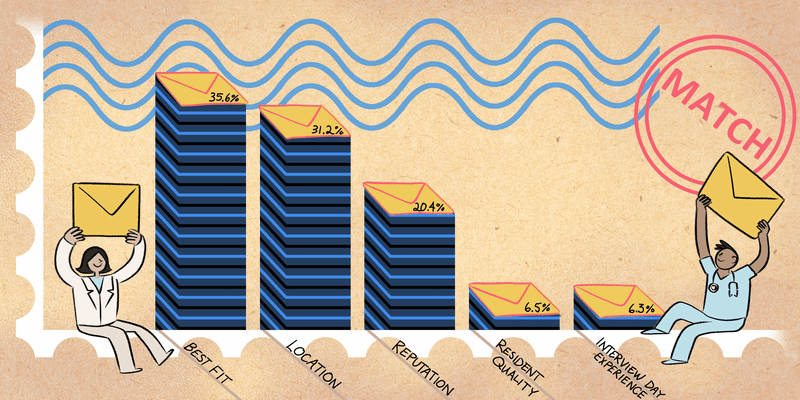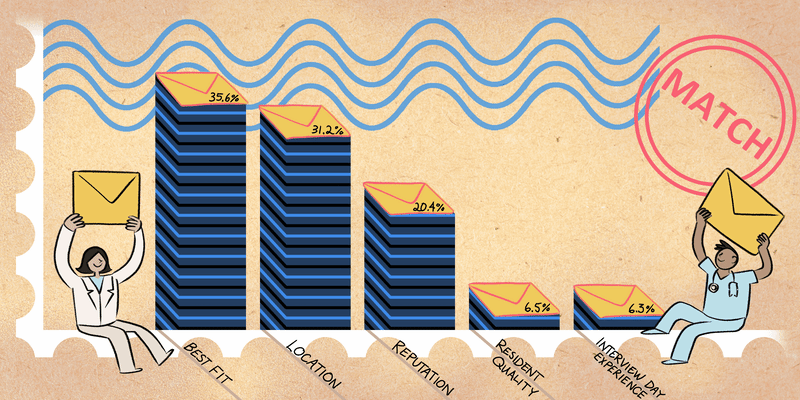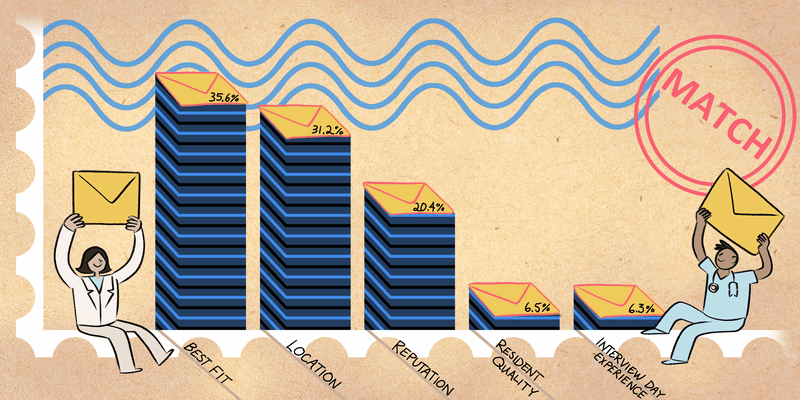
I presented a paper that my colleagues and I published. We described how heart centers for women evaluate ischemia. Since women often present with chest pain with no obstructive coronary artery disease, coronary functional testing is often needed to assess the different etiologies of ischemia. Angina with no obstructive coronary artery disease (ANOCA) is found in women and men but is usually only evaluated by Women’s Heart Centers at high-volume academic medical centers. Given the prevalence of ANOCA in both sexes, Smilowitz et al. emphasized that there is a need for increased access to physicians who are knowledgeable about ANOCA and its management. More cardiac catheterization labs need to expand their services to evaluate for ANOCA to improve adverse outcomes in female and male patients.
Another important topic at the conference was heart failure in women. Heart failure with preserved ejection fraction (HFpEF) is more often the etiology of heart failure in women, and new guidelines and consensus statement papers have just been published to address the treatment of patients with HFpEF. The 2022 heart failure guidelines recommend SGLT2is for patients with heart failure with any ejection fraction. The 2023 consensus statement paper emphasized that for women with heart failure symptoms, at any EF, women should be treated with SGLT2is, mineralocorticoid antagonists (MRA), and angiotensin receptor/neprilysin inhibitors (ARNI). Men benefit from MRA and ARNI only if their EF is <55%.
Diseases that involve small vessels, microvasculature, or endothelial dysfunction have a higher prevalence in women than in men. Pulmonary hypertension, HFpEF, stress cardiomyopathy, ANOCA, dementia, and cardiovascular diseases in systemic lupus erythematosus are examples of these. Research studies are needed to study the treatment of the microvasculature of these diseases to assess their benefit in these diseases.
Maternal mortality in the United States is the highest of all industrialized countries. Over forty percent of maternal deaths are due to some form of cardiovascular disease. Cardiologists need to be involved in the care of these patients. Since this was reported in the Lancet, many healthcare organizations, cardiologists, and obstetricians have written papers, started registries, and increased efforts to have medical insurance coverage increased to one year instead of three months to mitigate this increasing maternal mortality in the United States.
The link between breast cancer and cardiovascular disease not only share common risk factors, but each disease or its treatment can worsen the other condition. Unfortunately, hormonal therapies for hormone-dependent breast cancer can increase the risk of adverse cardiovascular outcomes. Selective estrogen receptor modulators (SERM) such as tamoxifen can increase thromboembolism. Aromatase inhibitors (AIs), such as Arimidex, can increase the risk of cardiovascular events such as myocardial infarction, heart failure, arrhythmias, blood pressure, atherogenic lipids, and metabolic syndrome.
The next American Heart Association Scientific Sessions will be on November 16-18, 2024 in Chicago, where it all started in 1924. It will be a special one since we will be celebrating the 100th year anniversary of this great organization whose mission is to advance the health of all individuals and communities.
Dr. Volgman has no conflicts of interest to report.
Image by gmast3r / GettyImages