The parallels I have found between high-level competitive sports and a demanding career as a surgical physician assistant have not come as a surprise.
My body and mind cannot differentiate the etiology of the adrenaline rush. I am a 6-foot, 4-inches former professional athlete who thrives on a busy demanding schedule. I spent my entire childhood and early adulthood feeling like I needed to prove myself, win a competition, and be the best. I believe that my height, inner motor, and athletic potential fed a constant need to prove that I was as large in life as I was in pure mass.
Although I earned a Division I basketball scholarship to college and played professionally overseas, I never lived up to the potential I had set for myself. I spent every day of my youth from ages 12–21 training my mind and body to be an elite athlete. Hours spent in the gym, on the track or basketball court were never-ending. On paper, I reached great goals, but I was always the second off the bench and third in line for recognition. During these years, I learned how to play my role as the base of a successful pyramid.
After witnessing and surviving my sister’s murder at the hands of her boyfriend in 2001, I decided to “help others” and obtain my physician assistant degree. While grieving and recovering from PTSD, I worked as a pharmaceutical representative and obtained my post-baccalaureate credits to apply to PA school. In 2008, I graduated with my PA degree and was interning as a new mother to an infant and 2-year-old. It was no surprise to friends and family that I took my boards during Braxton Hicks contractions two days before delivering my second child.

Over the next 7 years as a new graduate and practicing as a Urology PA at Mount Sinai Hospital in NYC, I learned how to communicate with sick patients and their families. I learned how to care for others and pay close attention to detail. I took on autonomy with procedures, consultations, and management of acute and chronically ill patients with diligent humility. It was at this time, I realized that the success I was supposed to have as a larger than life athlete was actually training meant for my physician assistant career. I never passed up an opportunity to take on a new role or challenge. I learned that exposure to anything new was good exposure. The training for my current team took on a new and deep meaning.
I am now the clinical director and chief physician assistant at the Mount Sinai Hospital, Department of Neurosurgery on the upper east side of New York City and finally feel that I have made it to the National Championships for which I have trained so hard for all my life: I work alongside Dr. Joshua Bederson, a world-class chairman and skull base surgeon. I’m confident my Urologic journey molded my demeanor and temperament. I’ve spent hours each day juggling sick men with prostate cancer and women with life-changing incontinence, and discussing the rigidity of men’s erections and just how bloody one’s urine was. Neurosurgery was an adjustment to discussing brain tumors, seizures, plegia, adrenal crisis, and how long I thought a loved one would be in a coma.
I am very lucky to specialize in skull base and cranial pathology as over 90% of our patients are elective surgeries and after a successful surgery go home on postoperative day 3–5. However, for each patient, each surgery and each day feels epic and usually gut-wrenching. My role as a surgical physician assistant is broad and demands precision.
A typical week is twelve-hour shifts Monday through Friday and taking phone calls overnight and weekends. I manage national and international patients bringing their care to NYC. My direct patient care consists of consultations in the office, assisting in surgery, inpatient management, and postoperative and surveillance care. I manage every patient’s journey to the OR by obtaining proper radiology scans, medical clearance, and coordination with collaborating physicians. I usually grow to love my patients with each phone call and email leading up to and following surgery. I attend twice weekly Neuroradiology rounds, department grand rounds, monthly pituitary, and skull base rounds. I travel nationally and internationally learning from surgeons and teaching my craft.
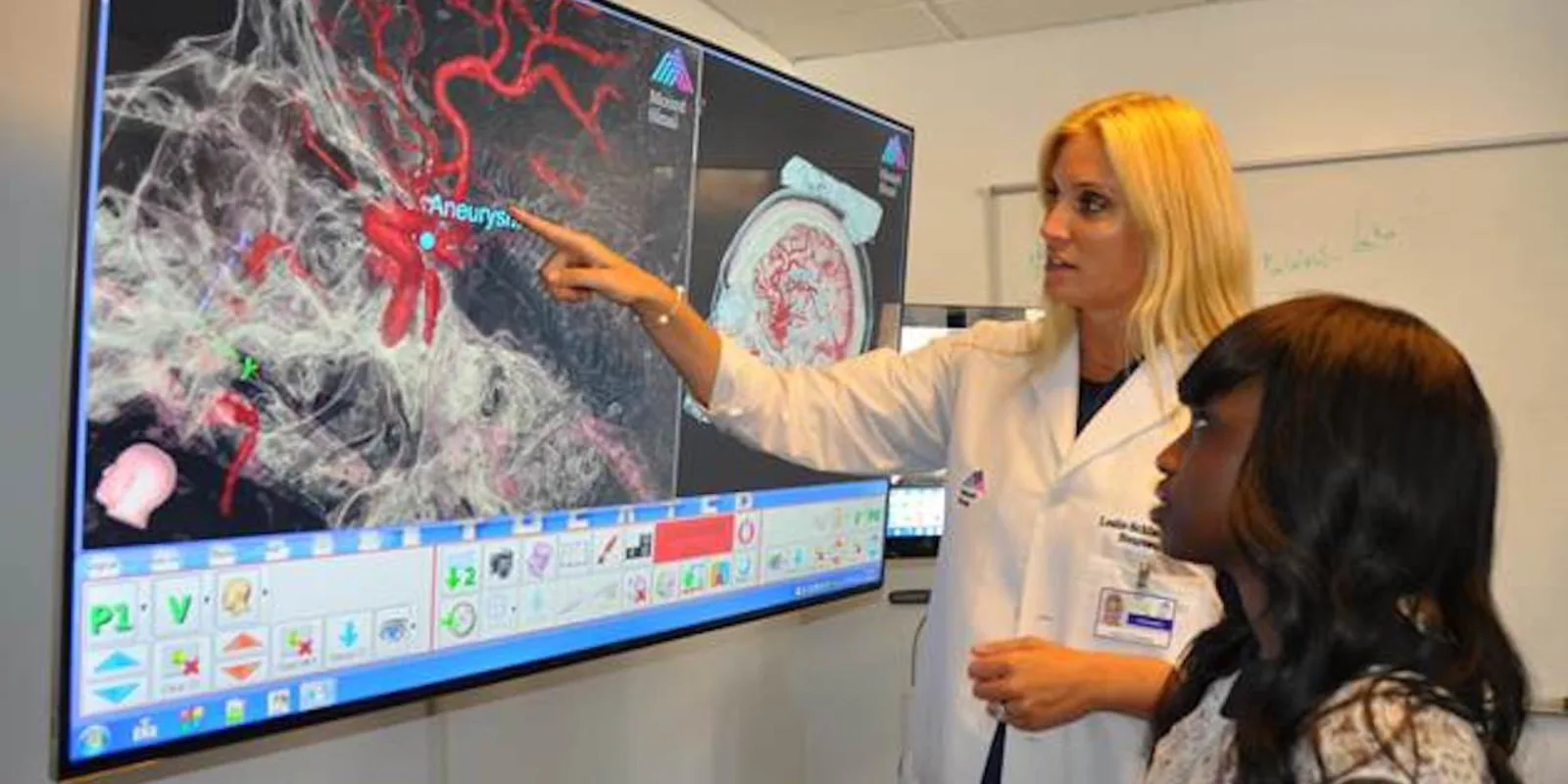
Cranial and skull base Neurosurgery at Mount Sinai hospital is performed by highly-specialized and skilled neurosurgeons along with a resident and often a physician assistant in planning and assisting. I have been lucky to specialize in preoperative planning, patient consultation and intraoperative navigation with advanced digital technology in Neurosurgery. I use 3D, virtual reality, and augmented reality to plan and navigate surgery, thus improving the surgeon’s awareness and comfort in the surgical plan. Our operative team, the surgeon, PA, tech, RN, resident, anesthesiologist, monitoring team are all on the same page and function like a dedicated, elite Division I championship team.
This patient/practitioner journey happens multiple times per week and each is representative of a patient, a life and a future. The patient’s journey from the office, to the operating room, the ICU, recovery floor then home is an exhausting and emotional process for which I feel equally invested. Despite my best efforts, I will never desensitize myself from the emotions, desperation, and fear I see in my patients and their families. That is one of the things that make me perform at an elite level.
When I go home each day exhausted and sore, I get into bed and realize that my hopes and dreams of being an elite athlete, performing on the basketball court, partially came true. The only difference is that I now perform on a different stage, in the setting of a patient care ambassador to my neurosurgical community. I may not win any more championship trophies or gold medals, but my victories—combined with the satisfaction and fulfillment I feel in my heart and head—are far more valuable.
Leslie Schlachter, PA is the clinical director and chief neurosurgical physician assistant at the Mount Sinai health system in New York City. She is a hybrid PA as she focuses attention in the surgical outpatient, inpatient and operative setting. She specializes in advance technology with simulation consultations, preoperative planning as well as intraoperative navigation for cranial and skull-based neurosurgery. She lives in New York City with her husband and two children.