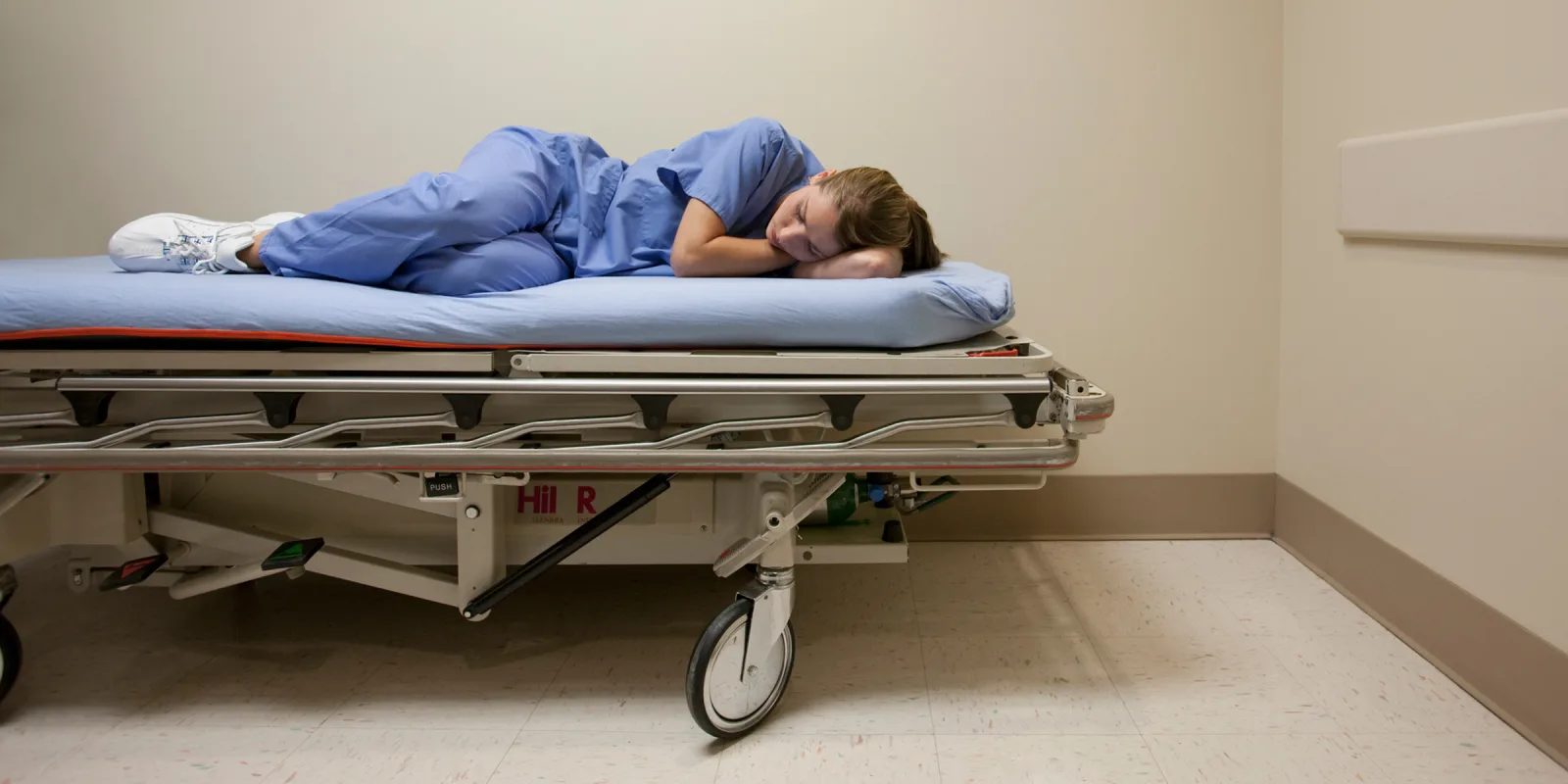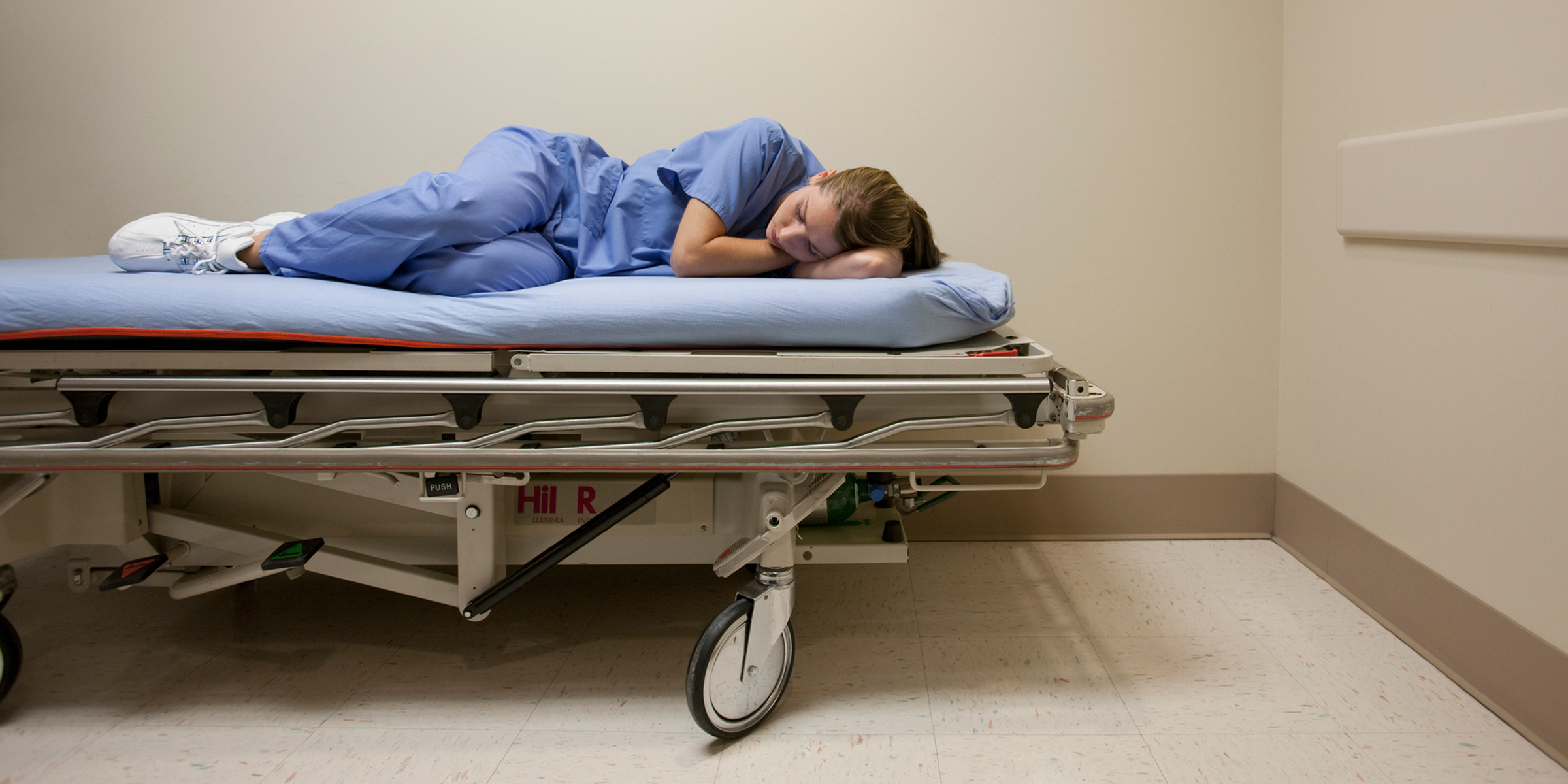
I write about a dozen work excuses a day. Migraine, fever, abdominal pain, ankle injury — I see all kinds of work-note worthy issues, but also some that I question. For example, take the young, otherwise-healthy patient who comes in because he injured his ankle the night before. I order some Tylenol and an X-ray. There is nothing broken nor dislocated; it’s just a sprain.
Then he asks: “Can I have a work note?” he asks.
"What kind of work do you do?"
“I’m a computer programmer.”
“So you sit in a desk most of the day?”
“Yeah.”
I proceed to write his work note.
Note: May return to work immediately.
Limitations: Keep foot elevated, use crutches for two days.
Signed, dated: Today @ 7:15a.m.
It's annoying to write some of these notes when I have personally worked hours on a broken foot, limping away, popping Ibuprofen for pain until I could take care of it at the end of my shift. One colleague went to work while enduring a miscarriage. She looked so miserable that a patient said, “Don’t take this the wrong way, but you look worse than I feel.”
Why do we do this? Why do doctors never call in sick (unless hospitalized or incarcerated)?
Doctors have a very strong work ethic — you are looked-down on if you are late, fired if you don’t show up. No other profession pulls as many all-nighters as ours during training (except maybe the military, which, by the way, also boasts an excellent work ethic). We go through 3–7 years of “boot camp,” during which we practice resilience by working 30 hours straight, often living off protein bars, and squeezing in 30-minute naps in smelly call rooms on hard cots. After those grueling years of residency, working a 12-hour shift without a break seems easy — even with continuous nausea from morning sickness.
Why do we do this?
We do it because if we call in sick, we’re letting our patients down; we’re letting our partners down. How can I call at 6 a.m. and tell the night-shift doc that I’ve been vomiting all night long, and I can’t come in? She worked all night with no sleep. At the end of that, few of us can even answer the phone, much less make life or death decisions (and I know very well that my “replacement,” if I did call, might not be available for hours, if at all!)
Thus, we bear it, and maybe we grin, too.
Some people have compared the airline industry to the medical industry when discussing safety and how we might improve safety in hospitals. If you are a commercial pilot, you call in sick the moment you get the sniffles because you know that piloting a plane requires your full concentration or disastrous consequences may ensue. You wouldn’t want a pilot that is impaired by illness (or the drugs that are treating that illness) manning the controls of your plane, would you?
Would you want a surgeon? An ER doctor?
Unfortunately, unlike the commercial airline business, which has a cadre of substitutes if you call in sick, doctors working at hospitals usually do not have that luxury. Is there a solution?
We must be kind to ourselves and our colleagues. We won't start calling in sick for the little stuff, but there should be a system in place whereby we can call in sick if we need to without the guilt of letting others down. In larger practices, an “on-call” system can make sick call-ins easier. In a small practice, this means relying on our partners. It is so important to build relationships of trust and mutual respect with each other. We won’t always be at 100% capacity at work. On the days that I just cannot find a replacement, I cannot close the doors to the ED. But I can have a strategy for those days:
- Self-awareness: I recognize I am not at 100%. I medicate in whatever way I can, don the mask, and wash my hands frequently.
- Admit vulnerability: I tell my staff – nurses, techs, clerks – that I am not running on all cylinders.
- Enlist help: Once I admit I'm not on my A-game, I ask my staff for help (“Please double check my orders, and feel free to question me. I need to be questioned today”).
- Slow down: Yes, I’m telling all ED physicians that when we’re not our best selves, we need to slow down so we can double-check things and make sure we’re making the right decisions.
- Err on the side of caution: Order the extra test, admit the patient, call the consultant. Obviously, it is not best practice to overdo it, but when we're not 100%, we are not making the best decisions and it’s probably better to practice more cautiously.
- Pray: I can’t tell you how many times I have prayed during a difficult day. I’ve heard that little voice in my head tell me to order the X-ray (found a new mass) or go ahead with that lumbar puncture (obtained frankly purulent fluid).
Some days following my strategy will work well.
Some days, it’s just a bad day and no strategy will help.
We really need community in our work, because what we do is hard. We need to talk to each other about these things and admit our vulnerabilities. Another voice I hear in my head (no, no, I’m not hallucinating) is that of Mel Herbert saying “What you do matters.” This is why we work so hard — because it matters.
Karla Newbold is an emergency physician currently practicing in Southwest Michigan. You can follow her at The Art of Medicine.