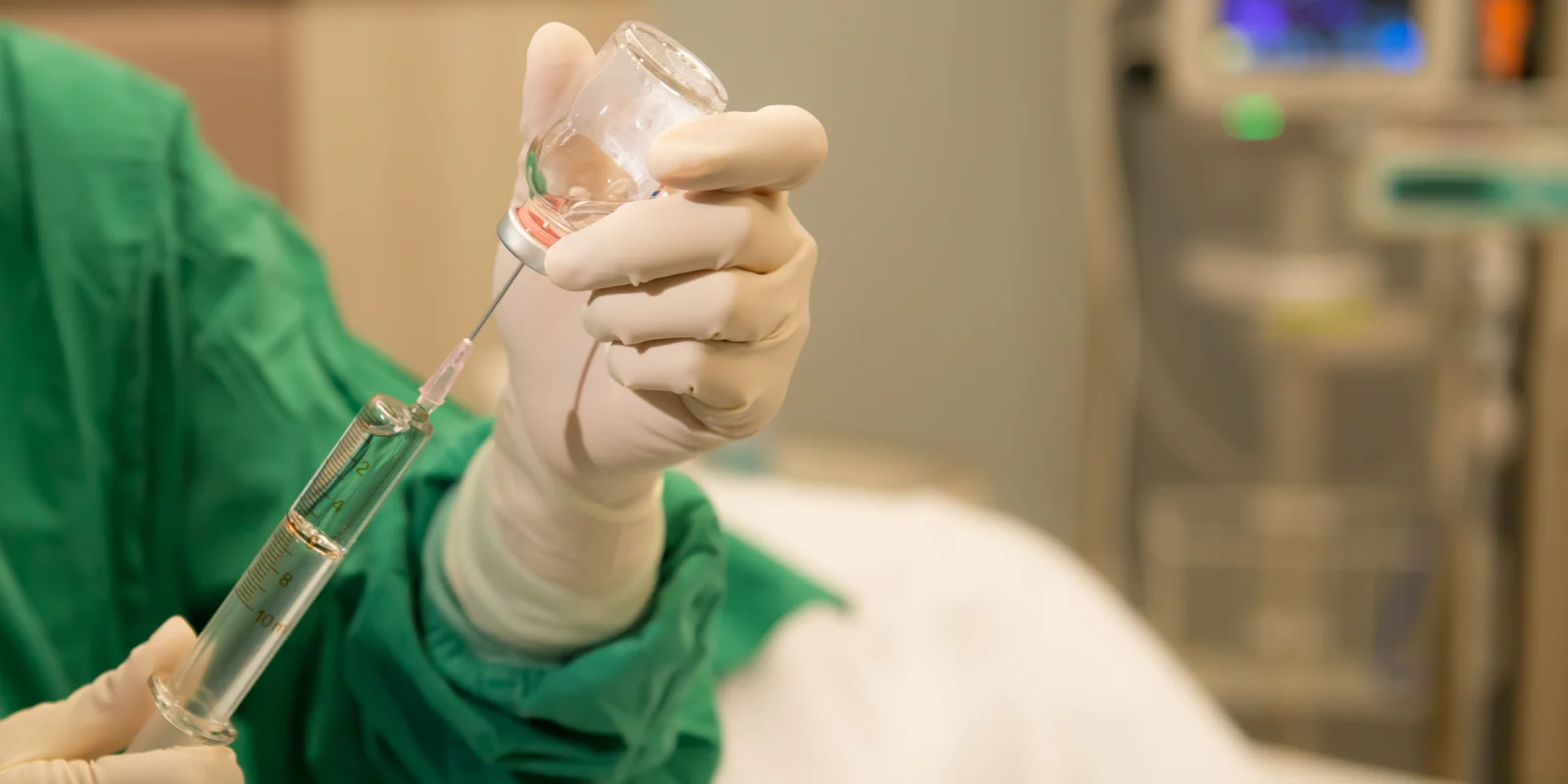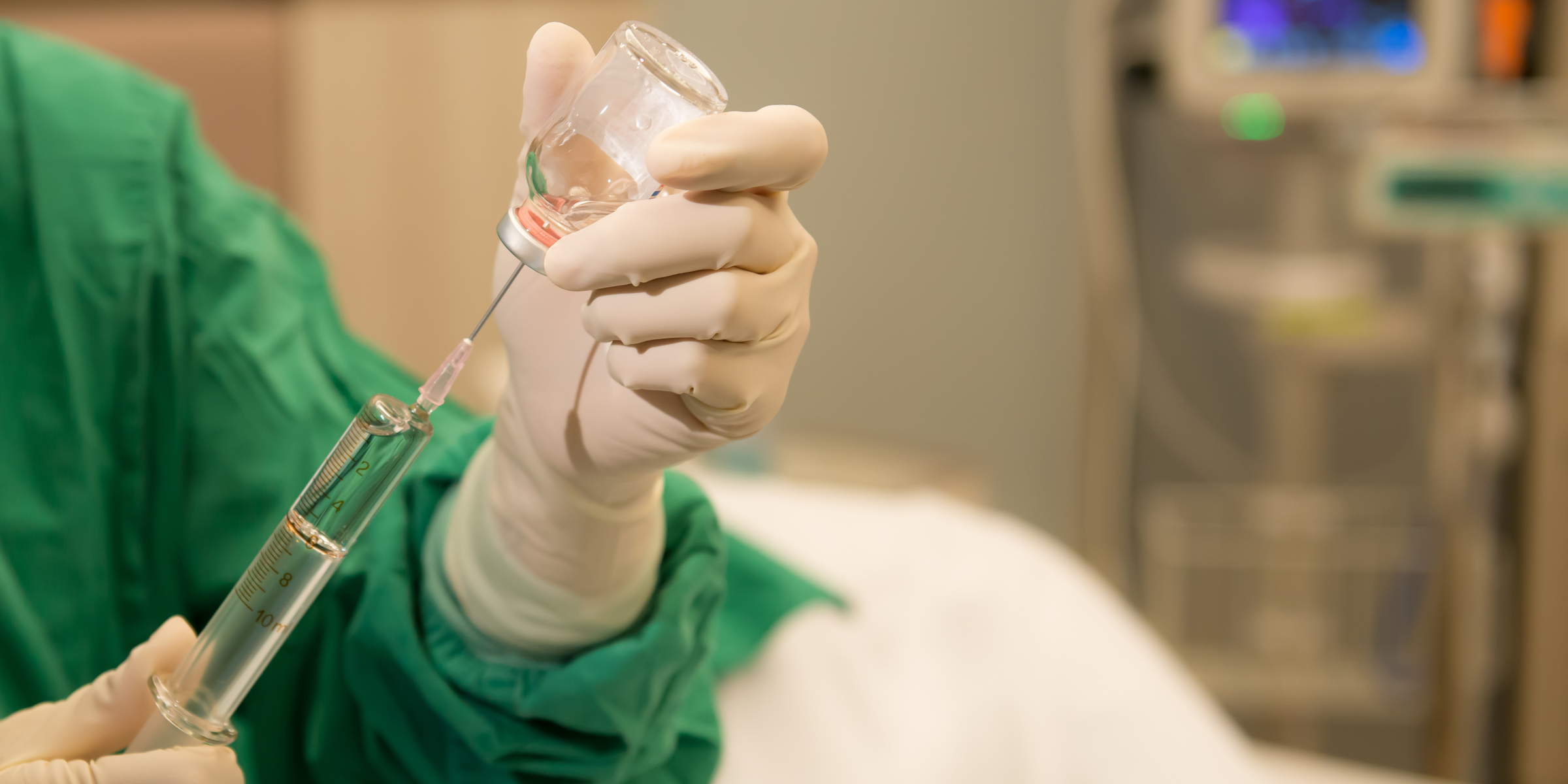
The radio barked and I walked over to my charge nurse’s station. We received a call for a middle-aged man with a self-inflicted gunshot wound to his left hand. Upon arrival, the patient, nearly in tears from his injury, politely greeted me with his uninjured hand while the affected hand sat in his lap, wrapped in massive amounts of blood-soaked gauze. His presentation was not unusual for Wyoming — cleaning one’s handgun before going to bed. Something “went wrong” and the firearm discharged through his hypothenar eminence. There was no OR availability until the next morning and even with 4 mg of IV hydromorphone, the patient trembled from excruciating pain. After extensive discussion with the plastic surgeon, we agreed that I should attempt a regional block. An ultrasound-assisted ulnar nerve block essentially eliminated his pain and he required no further narcotics on the floor prior to surgery several hours later.
I wandered into the adjoining trauma bay and found a 96-year-old woman who fell out of bed at her nursing home. Like all standard night shifts, not only did we fail to obtain ample history from the patient (nonverbal at baseline), we could not contact the skilled nursing facility and the emergency contact would not answer her phone. Her left lower extremity was exquisitely tender to any attempts at log roll. The plain film showed a left femoral neck fracture. I decided to go slow and gave her a “conservative” 12.5 mcg of IV fentanyl. Well, that was not well tolerated. Her respiratory rate plummeted, and she then required facemask oxygen. Later, I pondered if a femoral nerve block or fascia iliaca block would have proven less risky and more efficacious.
If you are like me, you are no stranger to pain control and its subjectivity in dosing, route, and efficacy. My initial approaches generally include acetaminophen, ibuprofen, ketorolac, orphenadrine, pain dose ketamine, and IV lidocaine. Should these fail, I try the usual suspects: morphine, fentanyl, or hydromorphone with some ondansetron. But I do wonder, “Shouldn’t we address pain at the specific site? Is there a better way of approaching a patient’s acute issue?”
Yet, if you are like me, you also find yourself lamenting, “I wish I would have paid more attention when they were doing those regional block presentations!” Well — I finally did pay attention. At ACEP 2019, there were many wonderful lectures, but I specifically focused on regional nerve blocks and ultrasound-guided nerve blocks from two presenters: Dr. Alexander Ebinger, MD from the University of Colorado and Dr. Arun Nagdev, MD from Highland Emergency Medicine. Each reviewed regional nerve blocks and best practices with overlapping materials. Their live imaging and procedure explanations created an easily understood framework that I plan on adopting in my practice.
Perhaps one important concept I gathered from both lectures was that a femoral block provides incredible analgesia for femoral fractures. Although femoral nerve blocks will not eliminate all pain, it is generally accepted that when the block is successful, it significantly decreases the need for IV opioids. This is particularly important when your 96 year old, nonverbal, patient with a femoral neck fracture has a low threshold for apnea, hypotension and delirium, among other complications. At our institution, we frequently find ourselves on the floor managing rapidly deteriorating patients. These blocks help prevent said rapid responses and help our orthopedists and hospitalists filter fewer calls at night.
Despite frequent concern about intravascular injection and systemic uptake, nerve blocks can actually help us prevent systemic toxicity. Occasionally, we find large wound areas that inevitably require toxic doses of regional anesthetics. My colleagues and I have the privilege of teaching rotating family medicine residents and medical students. Perhaps our most frequent “chalk talk” involves toxic doses of lidocaine. This is important to discuss before said learner inevitably enters the room, guns-a-blazing with seven syringes of lidocaine 2% without epinephrine, to inject an oilfield worker’s large forearm laceration. Alternatively, I find that blocks of the median, radial, and ulnar nerves work incredibly well for complex distal upper extremity injuries and lacerations.
I hesitate regarding certain procedures. For instance, I will admit to reluctance regarding an interscalene or supraclavicular block. These can be used for humeral dislocations, forearm/wrist injuries, and deltoid abscesses as these target the lower cervical and high thoracic levels (C5-T1). I understand there is a great use for them in the world of emergency medicine, but in my community setting, the inherent risks or injecting the vertebral arterially, blocking the phrenic nerve (causing elevated hemi diaphragm via paralysis) or causing a pneumothorax outweigh my perceived benefit.
As with all things that are “new” with emergency medicine, please ensure that your surgical colleagues —orthopedics, plastics, anesthesia, etc., are all aware and agree with regional anesthesia. When in doubt, it is always best to over communicate. Document your dosage, location and rationale. Mark and time stamp the site with a marking pen and consider signing with your initials that you have done regional anesthesia.
Tips for Regional Anesthesia
1. Be mindful of your needle tip. Avoid injecting the nerve itself. Rather, “bathe” the nerve in the numbing agent to avoid direct injury.
2. Go long! Start as distally as possible when blocking the region of the body at interest (i.e., for an injury in the median nerve distribution do the median nerve block, not the sub-clavicular).
3. Know your toxicities and antidotes. Local anesthetic side effects include muscle twitching, tinnitus, circumoral paresthesia, auditory hallucinations and disorientations. If severe, CNS depression, cardiac dysrhythmias, seizure and coma may occur. Benzos for seizures. Intralipid for systemic toxicity.
Image: ravipat / shutterstock