Hordes of new doctors are released into medicine every July 1st. Nurses groan, knowing they have just inherited a fresh batch of doctors. With bright white coats and untarnished attitudes to match, these new practitioners experience quite a few firsts on this day. The first time to introduce yourself as doctor, the first time putting an order in the computer, the first time realizing that you have no idea how to order something as simple as one dose of Tylenol.
I would imagine most doctors can remember details from their own inaugural July 1st. Mine was a Tuesday, a little over 3 years ago. My ER “shift” that day was more of an orientation and I didn’t have to pick up my own patients yet, just learn the system and hope for some excitement. Early in the day I witnessed my first code as a doctor. Actually, the attending tried to have me and my co-intern run the code, but fortunately a senior stepped in after seeing our wide-eyed stares and slack jaws. That unfortunately set us up for the next learning opportunity, which was informing a family that their loved one had died.
My favorite July 1st memory is doing my first procedure as a physician. A patient came in unresponsive and our chief resident was running the room, calling out orders and directing everyone’s efforts, then he promptly intubated for airway protection. The nurses and techs worked quickly and efficiently. Everyone had a job to do except for the few of us interns who were standing aside, trying to learn but not to get in the way. Suddenly our chief resident turned to us and asked, “Who wants to put in the central line?”
I would imagine all of us were mentally jumping up and down and crying out “Pick me, pick me!” Outwardly we didn’t want to seem overly aggressive and maintained some composure. We quickly discussed who had done more lines, who had already gotten a procedure earlier. We decided I would be the one to do it, so I stepped forward.
My previous experience with central lines was rather limited — I had witnessed two of them, performed zero. When my chief resident handed me the kit, I quietly told him I had never done this before, hoping he wouldn’t change his mind. He fortunately just continued by telling me exactly what supplies I needed and to get up at the head of the bed.
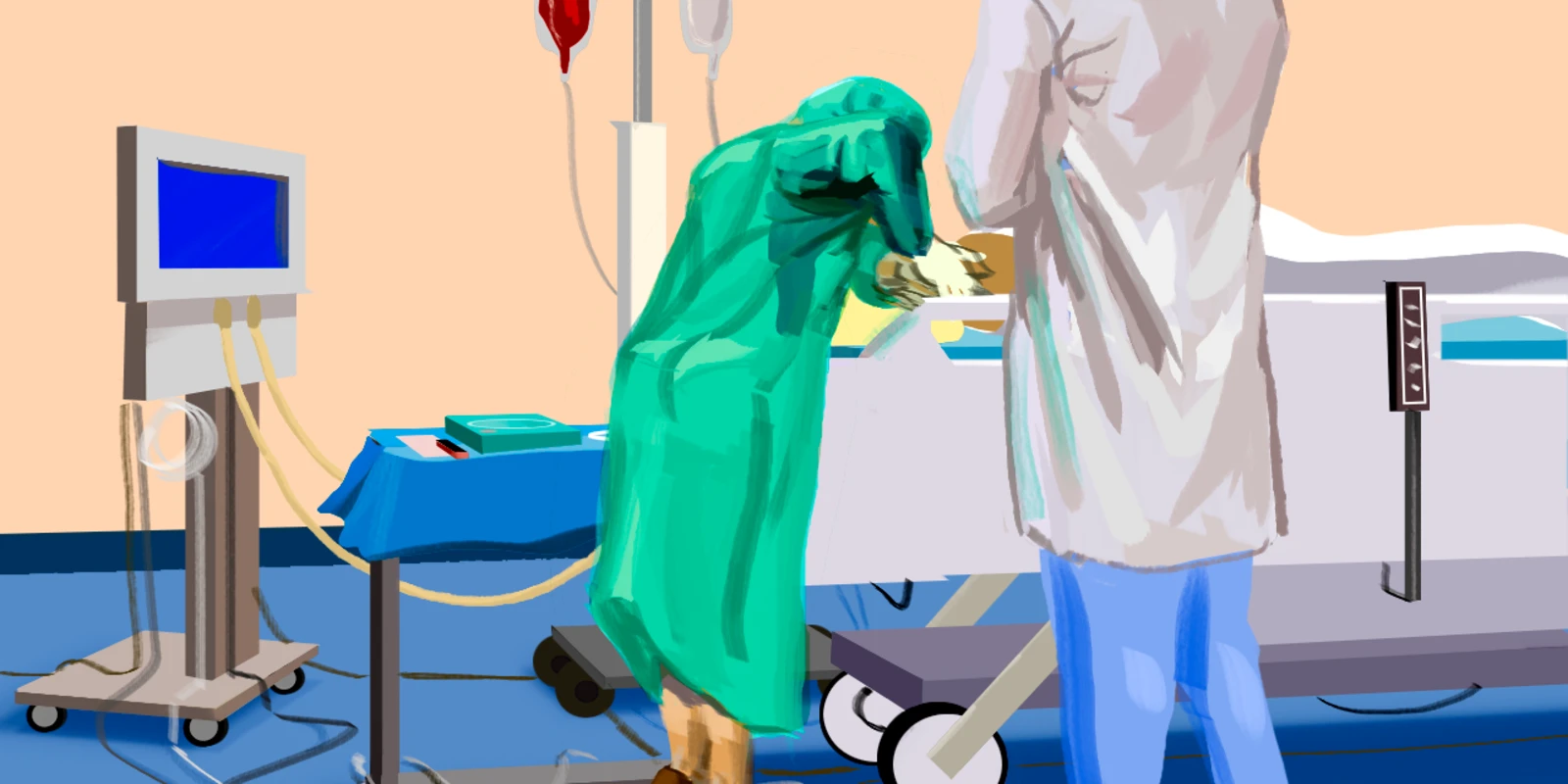
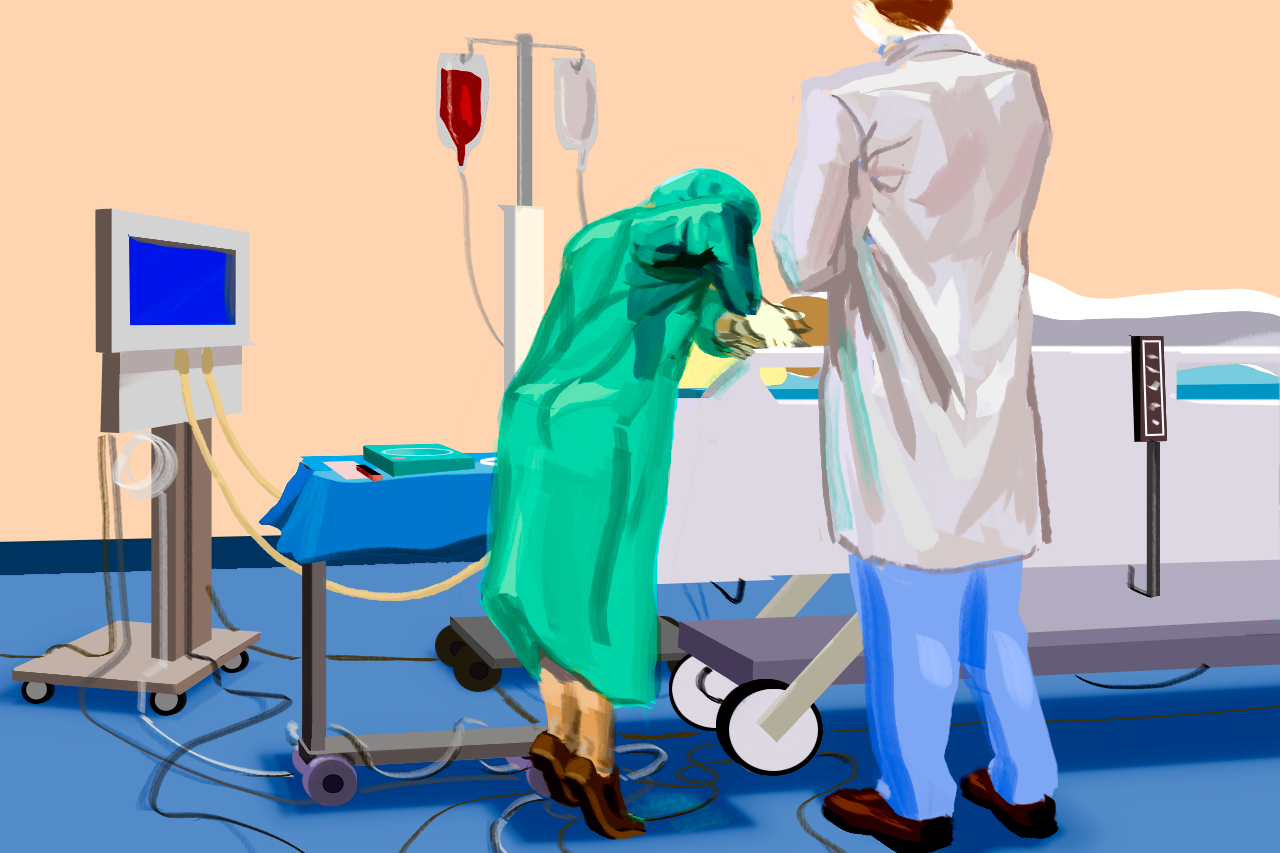
I gowned, gloved, and tried my best to stay sterile while weaving through wires and past the vent to get to the head of the bed without accidentally disconnecting anything. Then I saw that my chief resident was standing a few feet away with his arms crossed, no gloves or gown.
He talked me through the first few steps of draping and checking the equipment. With the preliminary work done, it was time to place needle to skin. I held the ultrasound as steady as I could, took the needle, and gently placed it against the patient’s neck. I saw the slight movement on the ultrasound screen, and looked up at my chief once again. He nodded, and again talked me through every small detail. Pierce the skin, don’t forget to hold negative pressure while you advance, almost there. I was so surprised when I felt the give on the plunger and saw the (thankfully) dark blood fill the syringe that I froze, but also because I had no idea what to do next. Again, he gave me clear step by step instructions — put down the probe, detach the syringe and have some gauze ready, thread the guidewire but don’t ever, ever let go of it. This continued through the very last step of the procedure.
After placing the dressing, I stepped away and almost fell over amidst the tangle of leads and vent tubing as both of my calves cramped into little balls of agony. Only at that point did I realize I had completed the entire procedure while standing on my tiptoes. My chief resident was about 6’4” tall and the bed had been set for him to comfortably intubate. When I stepped my nervous 5’4” frame up to the bed, I was so focused on the procedure and not messing up that I apparently compensated by standing on my tiptoes instead of thinking to ask to have the bed lowered.
I remember that my first day was a Tuesday, because I remember riding the elevator downstairs to our Wednesday didactics the next morning. My chief resident and another intern were also in the elevator, and I was telling them how I was so excited to go home last night and try to express to my non-medical field husband just how awesome my first day had been, including my very first central line. My chief resident just smiled as I thanked him profusely for the opportunity and his patience with me.
Fast forward three years to this past July, when I am now the chief resident and I am standing a few feet away from a new doctor, giving step-by-step instructions as she places her first central line. I’ve since learned that supervising a procedure is much more terrifying than even that first time doing it yourself, which gives me a greater appreciation for the patience I received from my own chief. I think back to that day and recall how nervous I was, so I try to pay it forward as I give directions: just a little bit farther, now pull back and don’t ever, ever let go of that wire. The procedure goes great and we both step back with relieved smiles.
Plus, she doesn’t know how good she has it compared to my first central line — at least we are both the same height.
Dr. Jen Bach is currently an Emergency Medicine resident in Livonia, Michigan. She will be relocating back to her hometown Grand Rapids after graduation this year. In her free time she likes to watch or play almost any sports, read horror books, and spend time with family. She has no disclosures and no conflicts of interest.