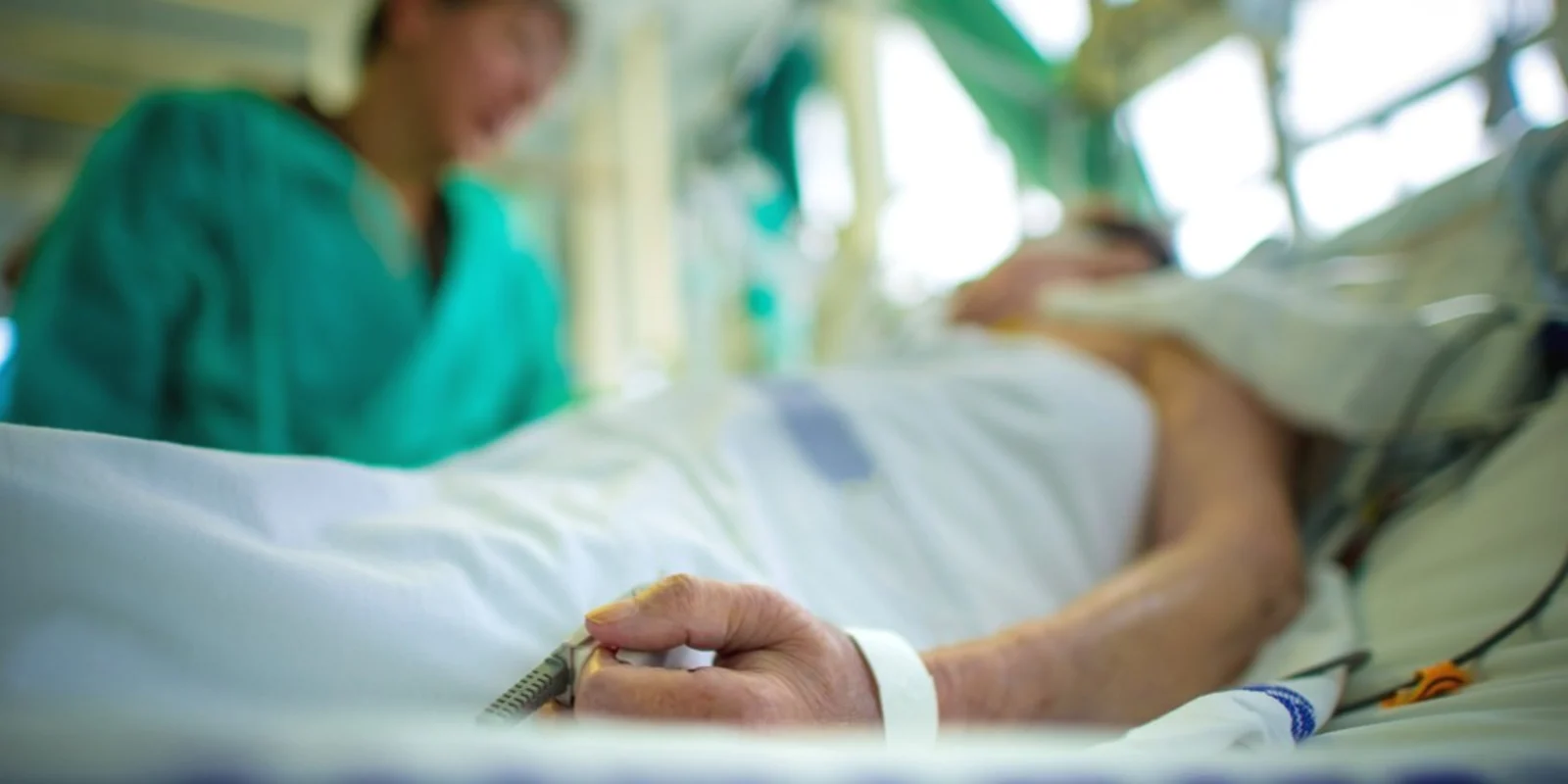
In the healthcare setting, empathy is defined as “a cognitive attribute, which involves an understanding of the inner experiences and perspectives of the patient as a separate individual, combined with a capability to communicate this understanding to the patient.” Clearly, an attribute like empathy would be hugely valuable in patient care. Yet, evidence shows that, as med students and residents train, they actually experienced a reduction in empathy.
There is an abundance of research on empathy in medicine. Diseker and Michielutte reported a decrease in empathy in medical students both prior to and after clinical experiences. Whitemore and colleagues reported that hedonistic personality patterns may contribute to this phenomenon_. Bellini, et al. used the Interpersonal Reactivity Index (IRI) to measure empathy of 60 residents at six points during their internal medicine residency training. They discovered that empathy only continued to decline. Lastly, Hojat, et al. found a reduction in third-year medical student empathy level when measured using a validated questionnaire, the Jefferson Scale of Physician Empathy (JSPE).
But, other studies have reached different findings. For instance, Zeldow and Daugherty (using the IRI scale) reported no change in empathy levels during medical school. In a 1979 study, Markham (1) found that a behavior science course during medical school made no impact on students’ perspectives of patients_.
Looking back at my own education, I consciously remind myself of my attitude when I started my journey into medical school. I remember writing my own version of the Hippocratic oath, and I recall an emphasis on empathy. Just recently, I opened the file to review on my computer. What a wonderful reminder of my commitment to medicine and patient care!
But as with all commitments, the pledge to empathy can use refreshing. With that in mind, as a physician, I do solemnly promise:
- to treat my patients with absolute respect, honesty, and transparency at all times
- to assist any person in need, regardless of age, race, financial standing, or sexual preference
- to exercise patience, sympathy, and empathy while listening to patient complaints with undivided attention and without interruption
- to remember the professors and mentors who provided me with guidance and the necessary knowledge to pursue this career
- to continuously supplement my education as I mature
- to support individuals of later generations who follow my example
- to keep patient information confidential and secure under any circumstance
- to refuse any temptation to commit fraud or to wrongfully gain unearned compensation
- to treat not simply the disease, but the entire person
- to provide reassurance and to establish a trusting rapport with my patients, their friends, and their families
- to never act superior and to treat both my colleagues and my patients as equals
- to seek help if I am unsure of the proper treatment in order to ensure the highest quality of patient care
- to personally apologize and admit my wrongdoing if I am ever to commit any mistakes
- to accept dishonor, disgrace, and poor reputation if I am ever to deviate from this pledge
- to experience satisfaction and gratitude while living up to these promises
I believe that providing targeted empathy training for students and interns would prove beneficial for both patients and physicians. In a time of rushed history taking and physical exams, I think that the establishment of an empathetic relationship proves undoubtedly valuable.
More medical schools are incorporating reflective writing, or “narrative medicine,” into the curriculum. Personally, taking a moment twice every month to reflect on my experiences and write about them has helped to re-center my focus on maintaining superior patient care. It is my goal to inspire other students, residents, and physicians to find a moment for reflection so that their empathy may endure.
Cherilyn Cecchini, MD, is a resident in general pediatrics at Children’s National Medical Center. With a future in hematology/oncology, her research interests include palliative care, communication during end of life care planning, and the concept of returning to normalcy near death. Dr. Cecchini has gained experience in narrative medicine by writing several pieces featured by the American Medical Women’s Association.
References:
- Markham B. Can a behavioural science course change medical students’ attitudes? J Psychiatric Educ 1979;3:44–54