Name: Peggy Finston, MD
Specialty: Psychiatry
Education: Yale University School of Medicine, Georgetown University Hospital, University of Pennsylvania Health System
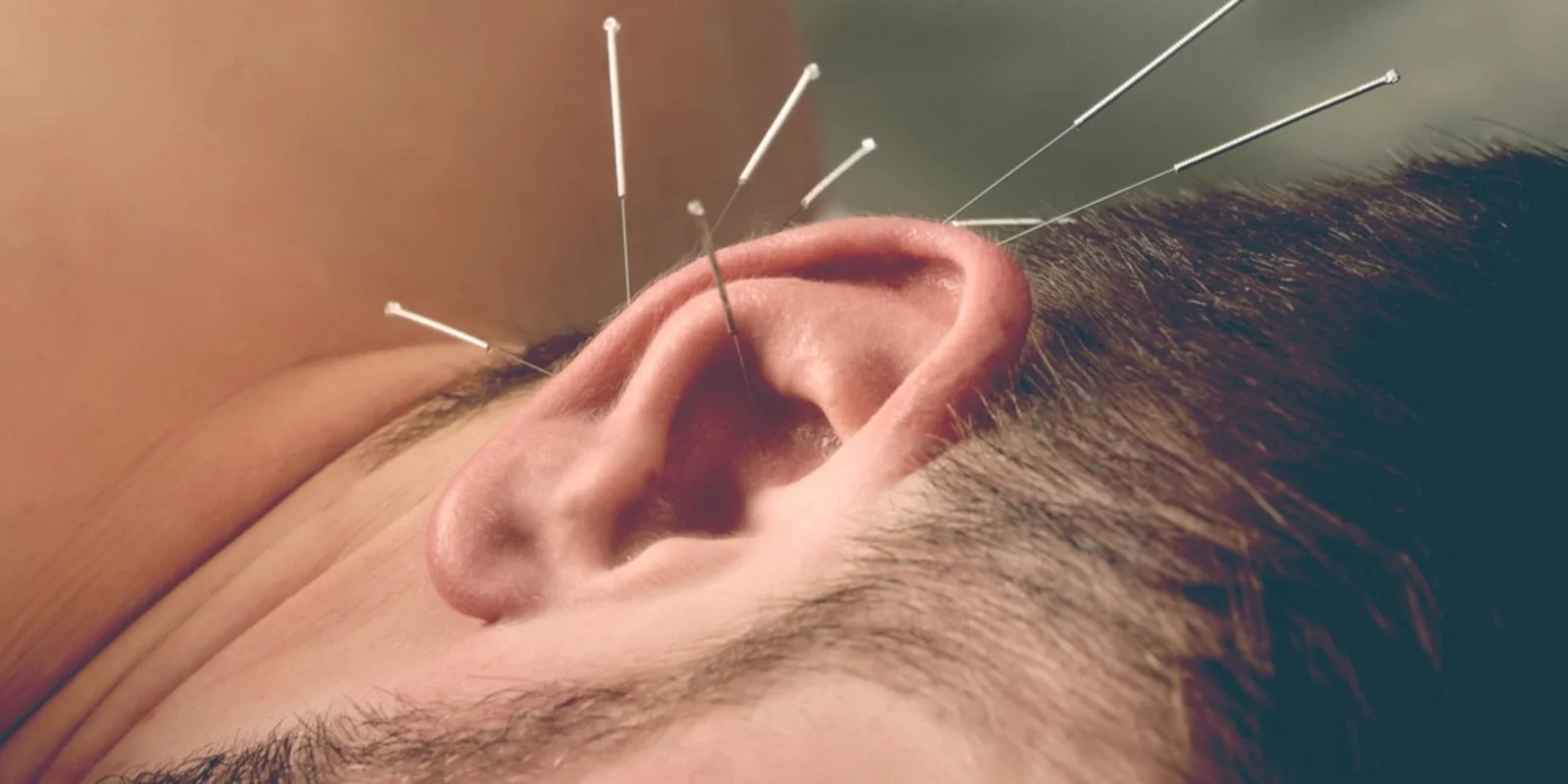
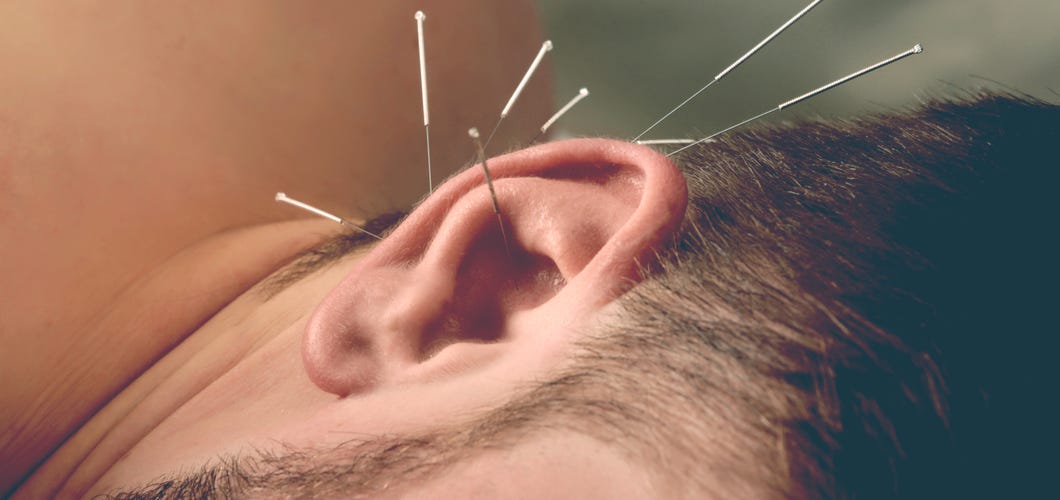
Areas of Expertise: Psychiatry, medical acupuncture
Current Position: Private practice
1. Why did you choose to specialize in psychiatry?
My family was working-class with no college graduates, no doctors, and no one telling me to become a doctor. Yet I was drawn to this specialty by age 7 or 8 and never seriously considered anything else. Some passions don’t come with reasons.
In my thirties, I visited a Greek Island, walked through the markets, saw the young women weaving rugs and blankets. Years later, I saw similar scenes in China and India and realized how fortunate I was to be born in a country where people with little could imagine and make some dreams happen.
2. What is a common misconception in psychiatry?
Most think psychiatry is a “check-box/med-check” medicine. Sadly, this is not a misconception for many practitioners today. There is no choice about this at most facilities. When I work at a new one, staff is generally surprised I actually talk to patients.
I trained in psychiatry at a time when doctors did talk to patients and aspired to be the potential catalyst for healing. The emphasis was how to cultivate a doctor-patient relationship to motivate hope and vision for themselves.
Psychiatry could and should be far more ambitious today. Instead, the emphasis is on looking for technologies that short-circuit the doctor-patient relationship.
3. What are your research interests?
The Star D Studies established that about two thirds of patients either don’t respond to antidepressants or don’t tolerate them. About half of those who respond will relapse within a year. In my acu-psychiatry practice, I focus on novel approaches for those who don’t respond.
I combine acupuncture and other energy balancing treatments with medication and psychotherapy. For example, one woman with bipolar had been hospitalized several times a year for years, with suicide attempts. Adding ear acupuncture every three months I see her, along with home treatments, she has avoided hospital stays for a year now. Her meds are the same. Her Raynaud’s has also has improved.
I also work at a local inpatient unit. There, I search for gaps in current approaches that might improve results. For example, normal thyroid studies do not exclude thyroid deficiency as a cause of depression. Peri-menopausal women who have insomnia, anxiety, depression and even psychosis may respond to estradiol supplement, etc.
4. Outside of your daily practice, do you have any personal or professional projects that you’re passionate about?
I have been composing music for 20 years, and recording my songs for the past ten years. Music has a profound influence on mood and memory. We remember the lines we sing and they may even guide us to better choices.
Our media culture encourages many negative behaviors. I try to write songs that are reflective and invite listeners to think about their own choices. Last year, I released my second EP, “My Soul UnCertain” available on Amazon, iTunes, and CD. A month ago, I released a single, “Dream Makers.”
5. Who are your mentors?
My first and actually only mentor was the psychiatrist I studied with during and after residency. Now, 40 years later, my mentor is me.
Like my first mentor, I frequently consult fields outside psychiatry to expand my grasp of human nature. My specialty provides a certain lens of “what’s wrong” to reach decisions about patients, but insufficient breadth to sense motivation and behavior. My study of acupuncture led me to read more about Chinese Medicine, and that led me to Torah texts. These disciplines deal with the soul as a reality and not a new-age construct. When patients are desperate, as in suicidal, that’s who you want to “meet.” There’s no check-box for that.
6. What has been your most gratifying moment of being a doctor?
I always get a thrill when I try a new treatment and it works, at least for that time. Recently, I applied a Chinese essential oil to acupoints on a man who had been depressed 40 years, had failed most meds, ECT, ketamine, etc. He stopped sobbing almost immediately. A few minutes later, his red face turned flesh color.
Other moments include working constructively with couples and families, and sensing a patient’s move toward a more personal, less stereotyped relationship with me.
7. How do you unwind after a challenging day?
Generally, I am too spent to get into music or other creative activities. Instead, I binge-watch Netflix and Amazon, or get agitated with my favorite political podcasts. Those jar and propel me into a different universe.
If I have enough energy, I visit my granddaughters. There’s nothing like children to refresh one’s weariness. The 7-year-old and I play doctor. I am the patient. Her special treatment is squeezing pus out of me — spiritual pus. Her family is religious. She also delivers babies — the dolls she puts under my shirt.
8. If you weren’t in this specialty, what specialty would you do? If you weren’t a clinician what would you do?
I truly can’t picture myself in another specialty. If I weren’t a psychiatrist I might do more with my music.
9. What are your favorite Doximity features and how have they helped your productivity (Dialer, DocNews, Career Navigator, e-Fax, etc.)?
I like the variety of news pieces from other publications I usually don’t see. The scientific ones, like the Nature article about the brain lymphatic system may lead to possibilities about treatments.
Opinion pieces about how physicians perceived by the public are useful, along with the health advisory pieces for the public. Most important though, are the forum pieces where I get to read how other doctors think about the current climate. This has been assuring for me that my colleagues are concerned like I am, articulate and on top of changes I have not heard about. The contact with them, especially former medical school classmates has brought a healthier dimension to my frustrations.