I tell my residents often that 80% of what we do in emergency medicine is bread and butter, the routine hum-drum of the ED. Those of us who practice, probably any specialty, know that about 15% can be utter frustration and demoralizing. It’s that remaining 5%, and the randomness of its appearance in our day, week, or month that drives us. It is the point …of care. In emergency medicine, it can be that needle (aortic dissection) you just picked up in a haystack (of chest pain patients) or an invigorating successful protection of an anaphylactic patient’s airway. For many this 5% is the point of care. It’s why they care about their job, their specialty and the importance of the practice of medicine.
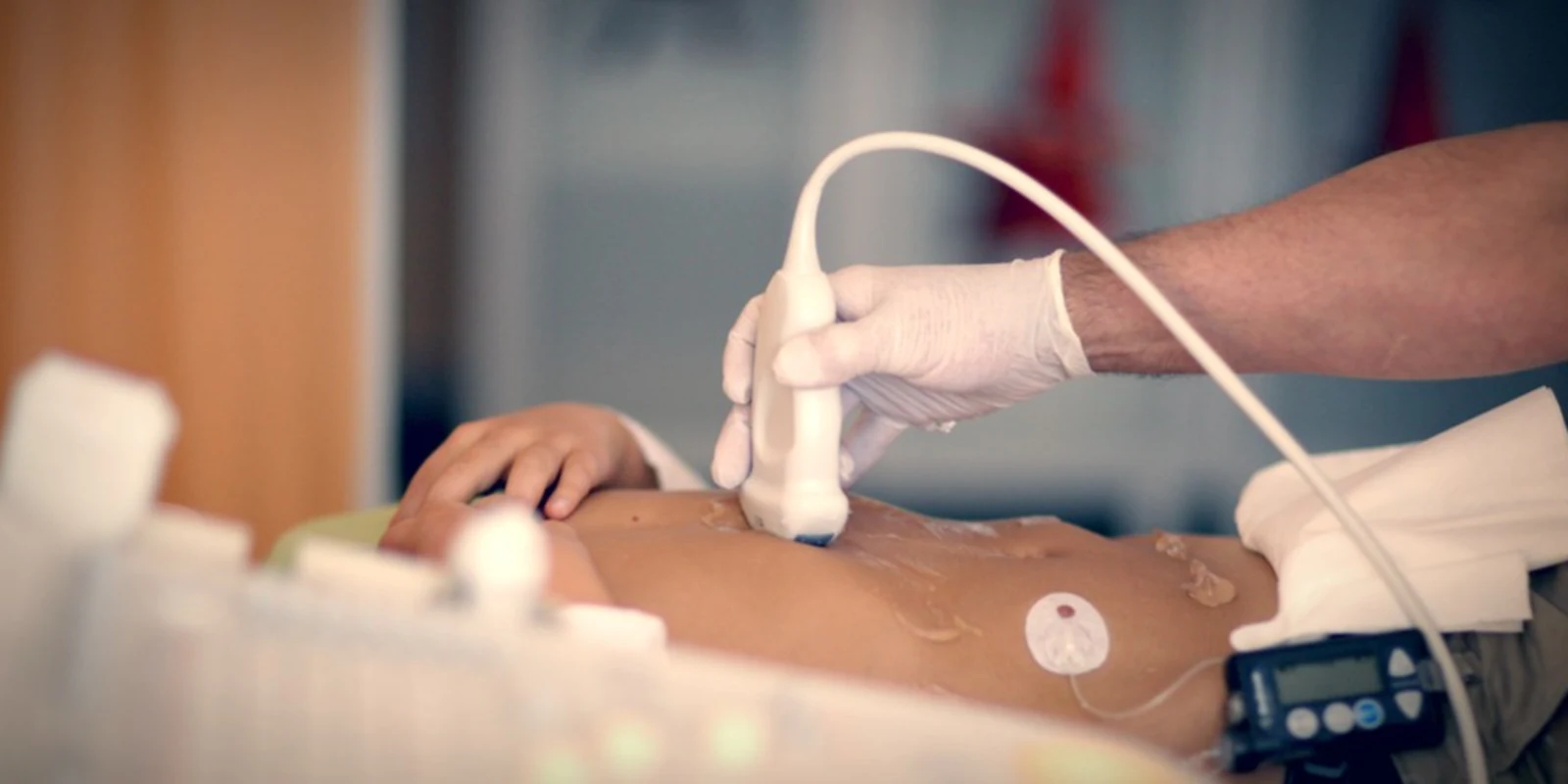
For me, an Emergency Physician fellowship-trained in ultrasound, I tend to agree. However, given the name of my sub-specialty “Point-of-Care Ultrasound,” there is a duality in the significance of the “point.” To me the point of care is both figurative and literal. Placing my hands and a diagnostic tool on the patient’s body, inspecting and probing his or her innards with my magical wand creates a connection long missing in the doctor-patient relationship. A relationship that has been shattered and distorted, truncated and separated by technology.
The electronic medical record and the house of medicine’s reliance on diagnostic machines — far away from the point-of-care — to tell us all that ails our patient has been a disservice to what many of them need the most. Patients need to be palpated, listened to, attended to, and to have their doctors spend some reasonable time at the bedside. This point — the physical contact and time spent pursuing concerning ultrasound findings — allows me to develop a bond of trust with my patients. Some studies are beginning to show the development of the patient’s trust and fulfillment when physicians use the ultrasound at the bedside.1 For those of us who practice this daily, we don’t need much peer-reviewed literature to know that it augments our holistic understanding of the patient and provides a nidus for the development of trust in what is normally a brief emergency department interaction.
Aside from improving our interactions with patients, using a diagnostic tool at the point-of-care opens doors to rapid diagnosis. Not by a digital robot, nor by a hard working radiologist tucked away in a dark room. For example, pressing on a firm rigid abdomen of a young women who was just wheeled into your ED, unconscious, alerts you as a physician to a broad array of potential diagnoses. We see cases like this often in the ED, and right after that physical exam I wheel over my ultrasound machine, as I ask the nurse for a stat IV and pregnancy test. Within minutes I have found a belly full of fluid, likely blood, and no evidence of an intrauterine pregnancy. I have narrowed down what was a broad differential within minutes without this sick young girl leaving my ED.
With my mouth I ask a history, with my hands I perform my physical exam, and with my probe I make critical diagnoses right then and there at the point-of-care. That, I presume, is the point … of care.
Jordan Chanler-Berat, MD is an emergency physician, resident educator, and Director of Emergency Ultrasound at The Brooklyn Hospital Center. He is also the founder of a personalized clinical ultrasound training company for physicians called The POCUS Preceptor.
-
Howard ZD et al. Bedside ultrasound maximizes patient satisfaction. J Emerg Med. 2014 Jan;46(1):46–53. doi: 10.1016/j.jemermed.2013.05.044. Epub 2013 Aug 12.