I have experienced mixed emotions since the emergency release of the first COVID-19 vaccine. I’ve thought about the historical context of racism and health care, especially how medicine helped build the foundation for racism. Physicians and scientists published papers purporting genetic inferiority and allowed discrimination to dictate the provision of services and care. Medical textbooks championed the false belief that race is genetic and even described treatment and management based on race. Medical students were taught this pseudoscience and some still believe in biological differences between Black and white patients with regard to pain. Disparities birthed from this racist medical infrastructure persist to this day.
As a Black woman, I thought about my ancestors who were exploited for the sake of medicine: an institution with no initial intent to serve or help Black people. The Black men of the Tuskegee syphilis study were denied treatment. Henrietta Lacks' cancer cells were stolen without her consent and helped advance medicine. Black women slaves were experimented on without anesthetics by Dr. J. Marion Sims, which helped him develop new obstetric techniques. Resurrectionists were hired by medical schools in the 19th and 20th centuries to steal Black bodies for dissection. The examples are numerous and substantiate the mistrust in medical institutions and vaccine hesitancy among Black people.
As a doctor, I've thought about the risk many of my physician and nursing colleagues took — and continue to take — as a seemingly careless world continues to live life as usual and disregard safety precautions. I've thought about the many hands I've held, and parents and family members I've comforted as they watch their loved ones get sicker before they recovered. I've taken care of patients from three months of age to 34 years old. I've watched them suffer from acute COVID-19 infections, MIS-C, and COVID-19 sequelae. Even now, the long-term effects of infection with COVID-19 are still unknown.
As a public health scientist, I've been so excited to watch modern medicine work so quickly to combat such a contagious virus via a vaccine. I've also been saddened by the spread of false vaccine information, conspiracy theories, and social media posts with alarming untruths. These theories and posts only increase fear of the vaccine, especially amongst Black people who are disproportionately affected by COVID-19. And despite all the misinformation, until recently, there was very little government spending and effort to produce widespread campaigns in minority communities about the importance of the COVID-19 vaccine.
I, like so many Black physicians, sit at the intersection of various identities that can sometimes provide conflicting emotions. Instead of relying on my emotions, I relied on facts and received both doses of the COVID-19 vaccine. But it wasn't easy; I credit my Black colleagues who offered reassurance and reminded me to look at the science.
I can breathe again knowing we are so close to beating this virus. I am so grateful for this opportunity. Simultaneously, I lose my breath thinking about how many Black people will again be left behind if we continue to refuse vaccination. Previously, the medical system intentionally left us behind. Now, our mistrust in medicine is preventing us from moving forward and widening the disparity gap.
As clinicians, it is our role to encourage patients to receive the COVID-19 vaccine and to mitigate these disparities. How we engage Black patients is important. My Black colleagues, I implore you: be vocal, be heard, and be seen.
Be vocal in your personal community and the community at large. Talk with your friends and family about why they should receive the vaccine — they trust you. Use your social media platforms to encourage vaccine uptake and highlight and address facts about the COVID-19 vaccine. Prompt vaccine conversations with those closest to you. Encourage your colleagues to consider the valid concerns of the Black community when recommending the vaccine to their patients. For your patients, spend time asking why they are hesitant, acknowledge medicine's abhorrent racially violent history, and address their concerns with facts. Urge them to get in line when it's their time.
Be heard in your institution. Encourage it to create a focused campaign on minority vaccine uptake. Call for a strategic plan to address vaccine access for minority communities served by the institution. Join, create, or encourage the creation of committees focused on understanding vaccine hesitancy amongst minorities, competently addressing vaccine hesitancy, and creating a vaccine campaign. These committees should include local Black community stakeholders. The investment will not go unseen.
Get vaccinated, then be seen. Share your vaccine story and pictures with everyone around you. Consider writing about your experience. Discuss any hesitation and side effects honestly. Discuss how you overcame your hesitancy to make the decision to get vaccinated and be open to questions. When you get the second dose, share your story again.
However, to be clear, Black physicians cannot, and should not, bear the burden alone. All clinicians should be advocates for vaccine uptake, especially in disparaged minority communities. But it is also important that Black clinicians are the most vocal in our communities, the loudest about the need for COVID-19 vaccination, and the most visible when we get vaccinated. When we are not getting vaccinated, it is noticed. When we express hesitancy, we sow seeds of doubt. Believe me, I understand the exhaustion, but I challenge you to be an example. Get the vaccine and continue to use your voice to encourage vaccine uptake in the Black community. And if you are hesitant yourself, acknowledge your conflicting identities, but let go of your emotions and consider the facts; the vaccine is safe. In the meantime, the medical community must continue working hard to rebuild trust to ensure Black patients won't continue to get left behind.
How do you engage your Black patients? Will you encourage them to get a COVID-19 vaccine? Let us know below.
Paula Magee is currently a pediatric critical care fellow. She completed the Commonwealth Fund Mongan Fellowship in Minority Health Policy and obtained her MPH in Health Policy from the Harvard TH Chan School of Public Health.
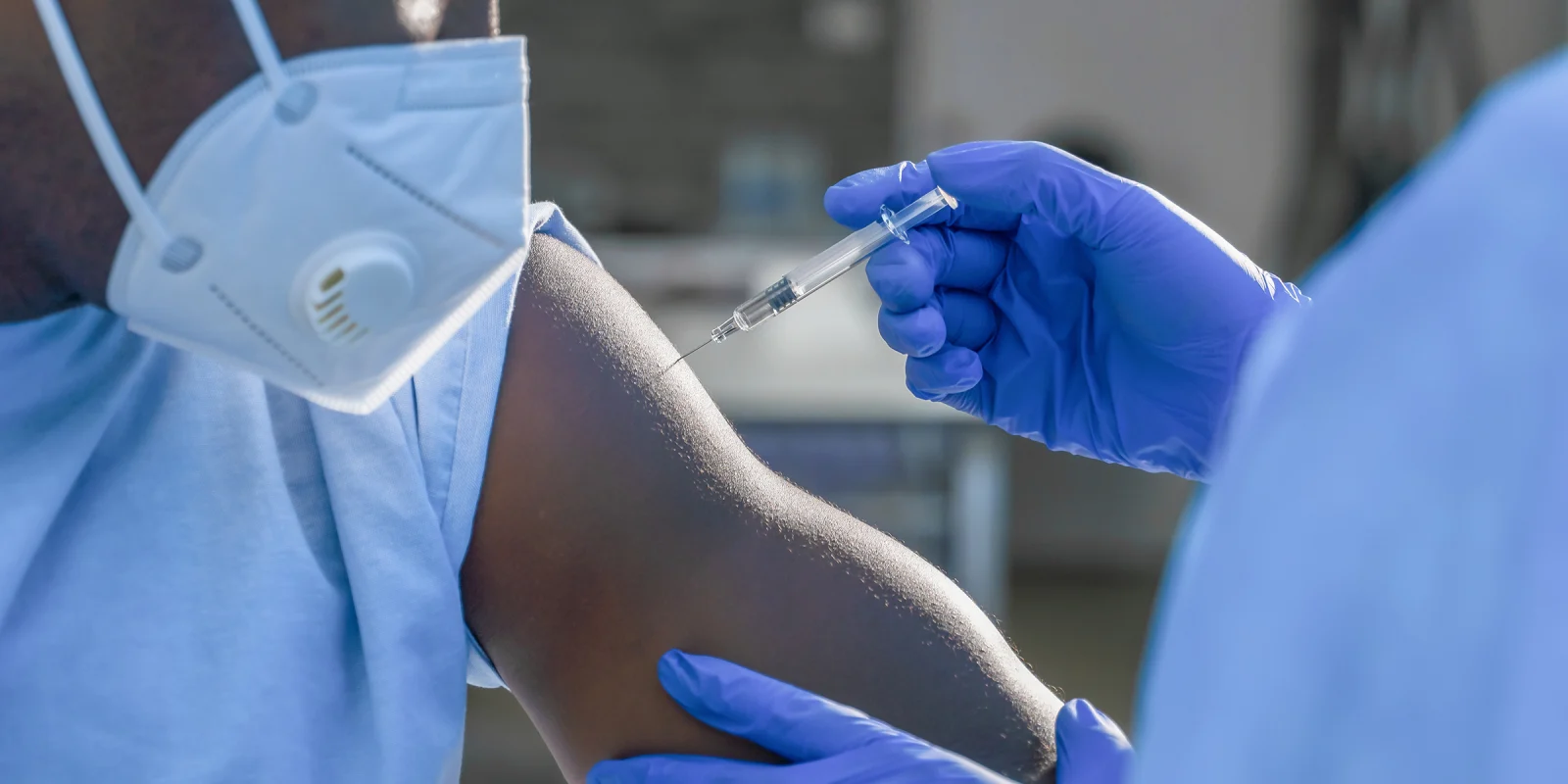
Image by Mongkolchon Akesin / Shutterstock