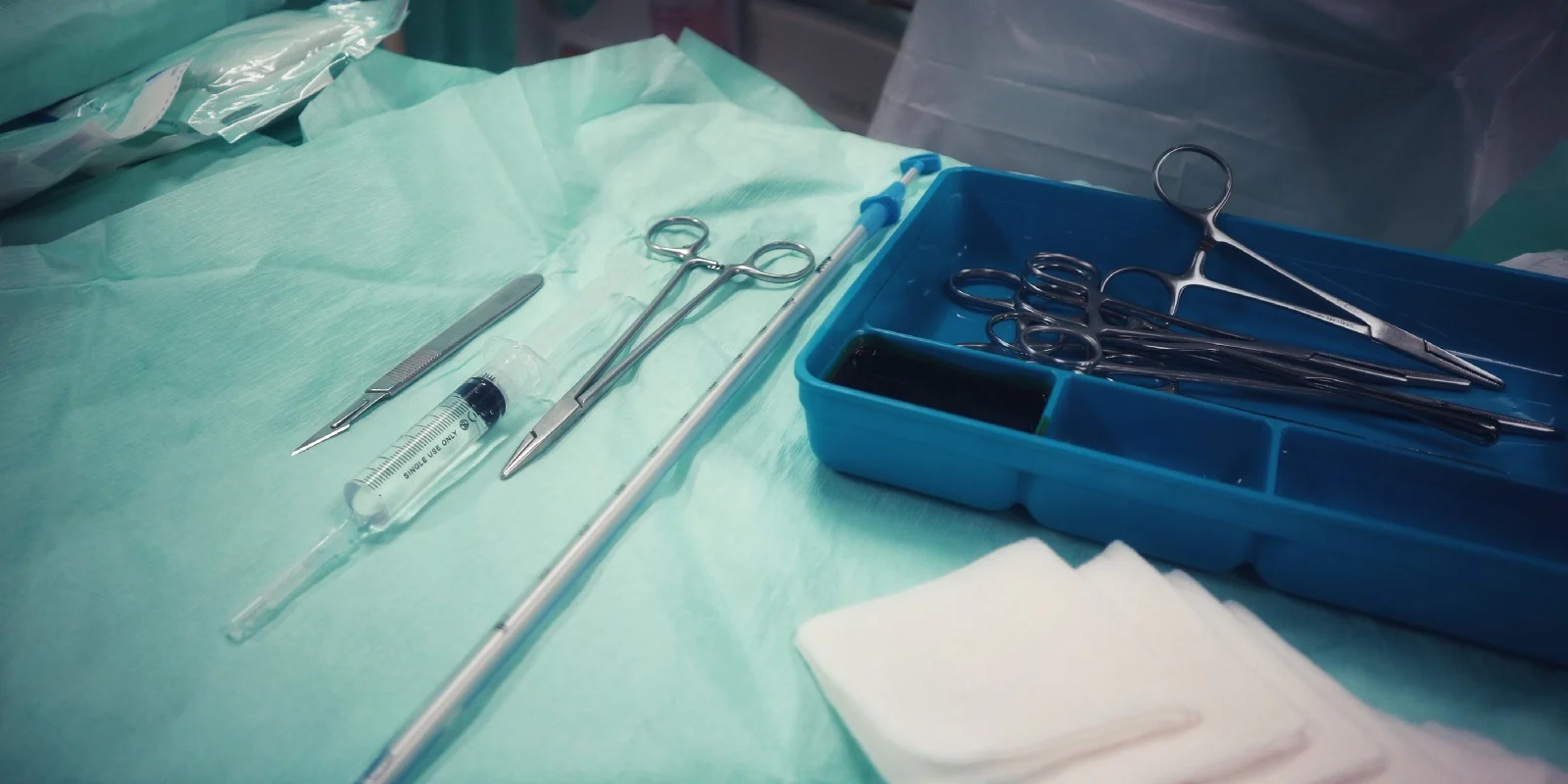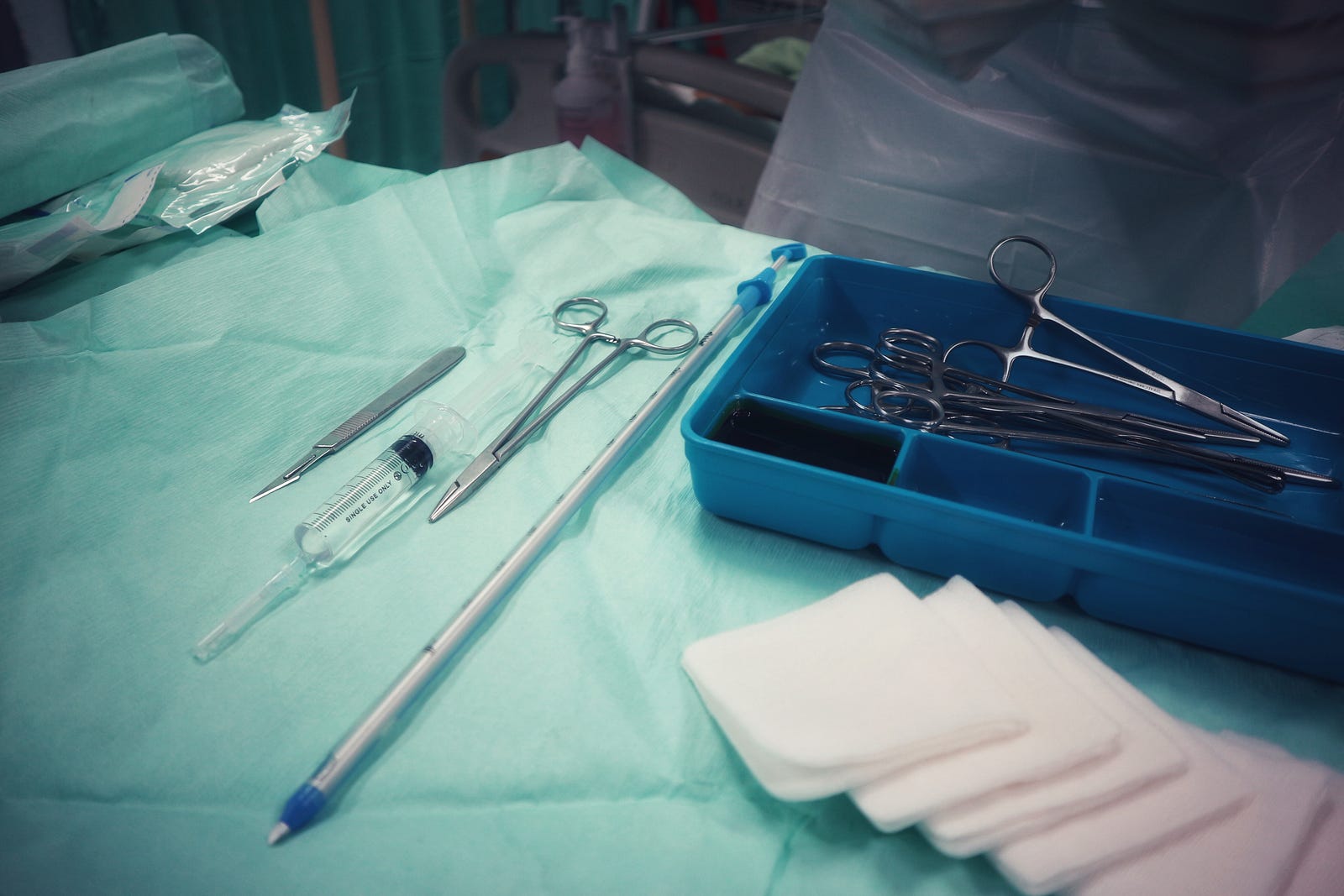
I was three months into an emergency medicine residency on a glorious late summer’s day when a fit 56-year old man arrived at the university ER complaining of chest pain and shortness of breath — not the cardiac kind but the pulmonary kind. While raking leaves when he had developed a sudden, sharp pain in the right side of his chest. The diagnosis was simple enough. A chest x-ray revealed a large, right-sided pneumothorax — big enough to cause pain but not big enough to threaten to his life. The mediastinum was straight in the midline, no shift, no tension. His vital signs were stable. This was before the day of pigtail catheters. In 1988, everybody with a pneumothorax received a chest tube. But who should do it — emergency medicine or surgery? No one thought to ask the patient his preference.
In teaching hospitals, turf is important. Mr. M. was stable enough to wait for a surgeon, but that would mean giving away the procedure. While surgeons aren’t particularly happy to have their rounds interrupted for an ER case, nor are they thrilled when asked to to baby-sit a patient after the teachable (and billable) procedure has already been done. The decision to place a chest tube was above my pay grade. Fortunately, the attending physician working that day was also the program director. He gave me the go-ahead. There was only one problem — I had never put in a chest tube. No worries. Marylou, another first-year resident, was fresh off her trauma rotation. She’d walk me through it, leaving our attending to run the rest of the department.
The see one, do one, teach one maxim can still be heard bouncing down the corridors of the nation’s teaching hospitals, meaning that inexperienced doctors are still performing procedures with little or no supervision on generally uninformed patients. There is a widely held perception that the best medicine is practiced at the nation’s academic centers, and it’s true for a good many things, but not when it comes to medical procedures during the summer months, when the interns are as green as the dew-covered grass at sunrise. It’s especially during these months when not knowing what you don’t know can hurt your patients. And yourself.
Sedation for chest tube placement has come a long way since I was a resident. Then, it consisted of sub-cu lidocaine, and — if lucky — a bit of IV morphine. Mr. M. was unlucky in many ways that day. I gloved and gowned before prepping the right side of his chest. Next, I drew an imaginary vertical line down from his nipple and another horizontal line from his armpit, marking the intersection with my thumbnail as the correct insertion site. After a tentative poke or two of lidocaine, it was time to cut.
Other than incising a few abscesses, I had little experience with a scalpel. It’s true that no great skill is required to hold one or apply pressure to the business end of the blade; the patient’s skin will readily part with adequate pressure. Here, the difficulty is one of aesthetics, knowing that you are purposefully cutting into living, breathing, human flesh. This is not the cadaver lab, or even the OR. In my arena, patients are awake and hyper-vigilant. The challenge in the ER is rather more ambitious.
Scalpel in hand, I began cutting the skin and muscle atop Mr. M.’s rib. Whereas this should have been done with a single firm incision, my hesitancy led to a half dozen provisional nicks and scratches. Okay, firmer and deeper, and finally down to the rib. Exchanging the scalpel for a pair of forceps, the next step involved puncturing the pleura, the thick, tough, richly innervated membrane separating the pleural cavity from the chest wall. To get an idea of the force required, imagine poking a pair of blunt-tipped scissors through the palm of your outstretched hand.
Fast and forceful is the ticket, but my first attempts were feckless. Under MaryLou’s urging, I punched harder — a gasp from the patient and then a sudden rush of air against my fingers. Success! Now all I needed to do was thread the tube through the hole. I opened the tines and pulled back to create a larger rent in the membrane. Then a finger down the rabbit hole into the chest. Lose your finger, lose the rabbit. But I didn’t know that, and somewhere between puncturing the pleura and exchanging the forceps for the chest tube, I lost track of the hole. There was so much I didn’t know, including that a properly placed tube advances easily. So, when I slid the tube upward and met resistance, I just kept pushing, ultimately shearing the pleura away from its attachment to the ribs. The tube was superficial, not deep, and decidedly not in the chest cavity. Nobody — not the patient, not MaryLou, and certainly not me — realized just how badly the thing was being botched.
The ensuing chest x-ray appeared to show a perfectly placed thoracostomy tube except for one thing: the pneumothorax was still there. Having inflicted significant pain, I had failed to fix the problem.
My attending looked at the film.
“Call the cardiothoracic surgeon,” he said blankly.
I did and, to his credit, the surgeon didn’t chew me out. As he looked at the x-ray, I asked him what he thought of the tube placement. His response was simple: “It doesn’t matter that the tube appears to be correctly placed — all that matters is that the pneumothorax persists.” And with that he took off his coat, rolled up his sleeves, and proceeded to properly place a new thoracostomy tube. The entire process took less than five minutes, and the ensuing chest x-ray was pristine; the lung fully expanded. The surgeon said nothing to me, but I couldn’t help overhear his comment to my attending. “You need to keep an eye on your boy. He doesn’t know what he’s doing.”
It’s true.
I didn’t and even now, thirty years later, the rebuke still stings.
It’s time to bury See one. Do one. Teach one. Let it sleep with the fishes.
Bob Clare is an emergency physician who lives in Tidewater, Virginia. After graduating from medical school from the University of Pittsburgh in 1988, he completed a residency in Emergency Medicine at the Eastern Virginia School of Medicine. In 2010, after a long tenure with Emergency Physicians of Tidewater, he saw the light of independent contracting and now work as a “local locums” at several hospital emergency departments in southern Virginia and North Carolina. He maintains a medical blog intended for a general audience at http://skepticalep.com. An avid inline speed skater, he spends his spare time skating, running, and cycling. He reports no conflicts of interest in the writing of this article.