 In order to successfully move forward, one should learn from the mistakes of yesteryear. When the AIDS epidemic appeared in the 1980s, the house of medicine was shaken to its core. Unfortunately, the novel coronavirus pandemic of 2019 has once again struck the house of medicine in ways never thought possible.
In order to successfully move forward, one should learn from the mistakes of yesteryear. When the AIDS epidemic appeared in the 1980s, the house of medicine was shaken to its core. Unfortunately, the novel coronavirus pandemic of 2019 has once again struck the house of medicine in ways never thought possible.
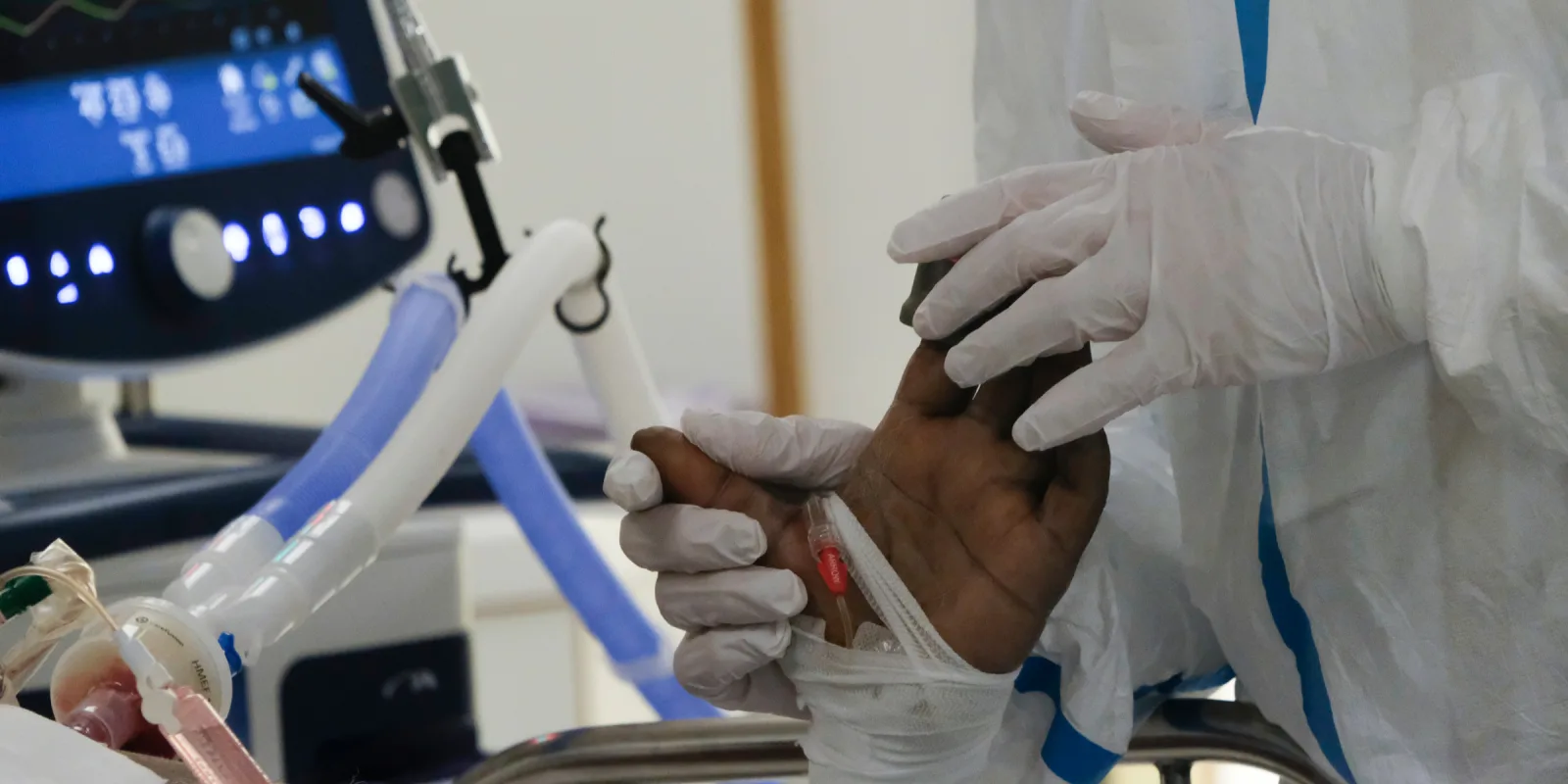
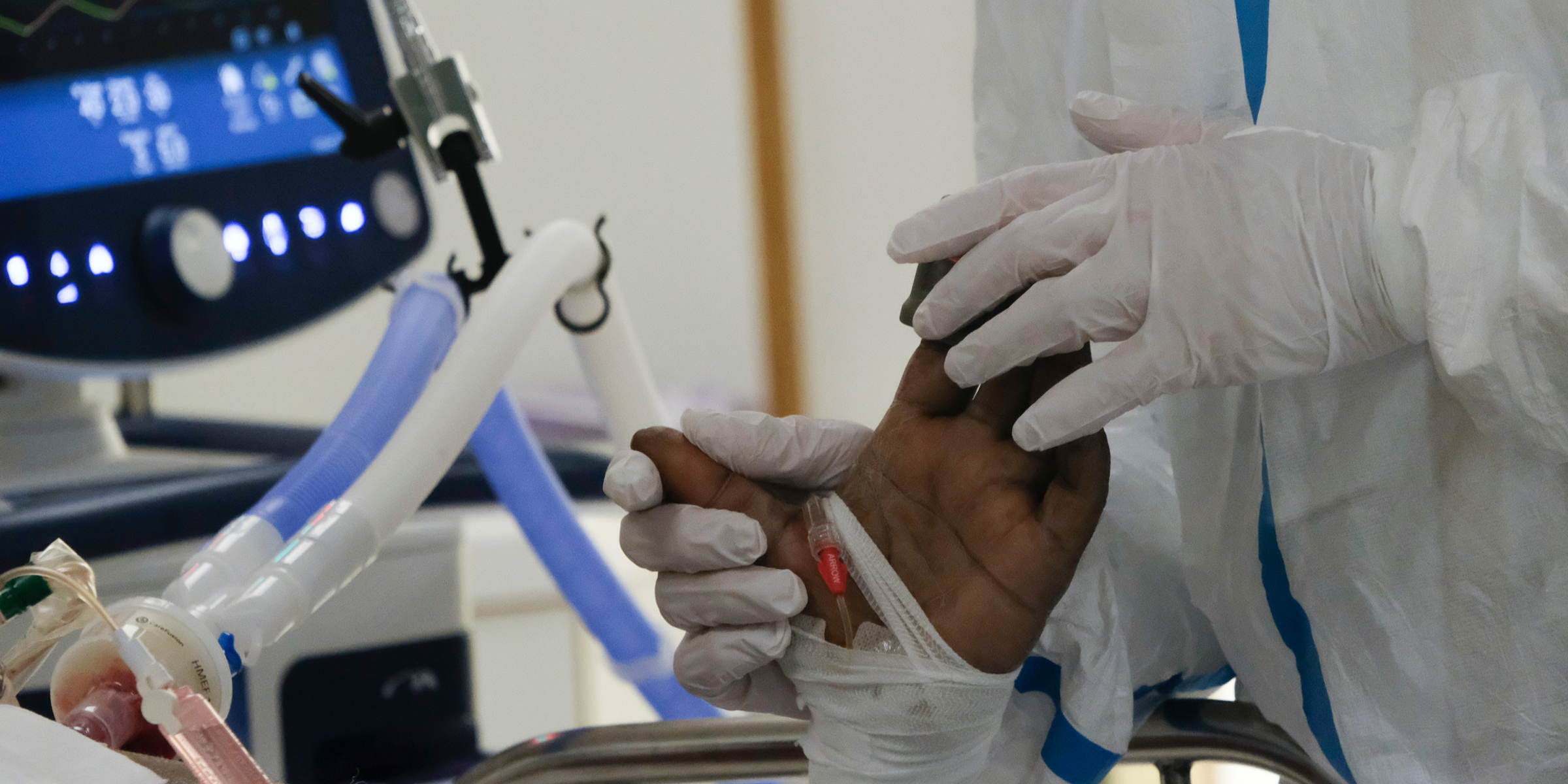
This current coronavirus pandemic has many similarities to the HIV/AIDS outbreak of the 1980s, though there are striking differences as well. During the HIV/AIDS outbreak, we were facing an unknown, potentially killer disease, with the (unfounded) fears that it was infectious just by being in the same room as an HIV-positive patient. Although we later found out that HIV was not as infectious as we feared, COVID-19 is proving to be one of the most infectious of the coronaviruses that has affected the human race. As a result, many health care workers have become ill and even died in the regular course of taking care of patients, despite “universal precautions” and the use of PPE. At the height of the HIV/AIDS crisis patients similarly presented in droves to clinics and EDs, and health care workers did not know how to initially care for them, except to offer supportive care. However, never did HIV overwhelm society to the degree COVID-19 has with hospitals overflowing with patients but without the resources to care for them, not to mention the economic collapse of societies around the world.
As we pass what is hopefully the pinnacle of the curve, we must now look to a changed world, not quite “post” COVID-19 — as experts have suggested it may stay with us for months to years to come — but to one where, like with HIV/AIDS, health care workers must return to the reality of working with COVID-19 infected patients and staff. People not immune to COVID-19 will need to follow the hard lessons of the “AIDS epidemic” by instituting and recreating a “universal precaution” protocol, until we have a proven treatment and/or vaccine. Our clinical experience in New York City showed us that the community spread of COVID-19 was so extreme that even unrelated trauma cases in otherwise healthy and asymptomatic individuals later revealed COVID-19 infection.
Indeed, it seemed you could not sprain your ankle in New York City without having COVID-19. Hence, in the world after, we must accept that community spread will continue and that asymptomatic COVID-19 patients may have other medical conditions to which the health care industry must attend. As federal and state governments grapple with timelines on when to open their respective domains, health care must resume its normal businesses urgently. Just as hospitals learned to operate and perform procedures and treatments on people with HIV by treating everyone as if they had HIV, we must do the same with COVID-19. Obviously, this will require a sufficient and long-term investment in PPE by hospitals, which must also not hamper the efforts of health care workers to supply their own.
Another lesson from the AIDS crisis was that testing is the key to containment and helps with prevention. In the case of COVID-19, our inability to provide sufficient early testing led us to lose the opportunity to contain the virus, and as a result, our only option was to attempt to mitigate the spread — the so-called “flattening of the curve.” If we are to move safely and responsibly forward, and before such a time when a vaccine or treatment is developed, we must develop sufficient testing capabilities to know who the carriers are and to expeditiously isolate them from the public. It may be prudent to implement rapid testing centers throughout society to correctly triage patients and not promote the dispersion of infection.
The general public must also move forward in the world post COVID-19 and accept their new reality. For the foreseeable future, handshakes may be a thing of the past. Wearing masks in public should no longer be something looked upon with disdain and suspicion and should instead become accepted as commonplace. Hopefully, we can increase production to overcome our present inadequate supply of surgical masks, hand sanitizers, and toilet paper, and businesses will be able to provide ample amounts to their customers and employees. Frequent cleaning and wiping down of surfaces, be they countertops, gym equipment, or public utilities, will now require full-time personnel to perform and likely need public compliance. Our elderly and vulnerable populations may still need to practice social distancing, but with everyone protecting themselves and doing the “right thing,” they will not need to be locked up in their homes in perpetuity.
We must learn from these mishaps and lack of preparation in order to make sure we are able to effectively identify those with COVID-19. However, we must continue to exist as a society by practicing the new normal of universal precaution against COVID-19. With time, the hope is that our scientists and biotech firms will develop treatments and ultimately a vaccine. Hospitals must also stop thinking shortsightedly in their haste to increase their medical staffing for the next crisis, only to cut their pay and lay them off when they realize they are no longer needed. As we now definitively know, the resurgence of another pandemic is only one mutation, one wet market, or one international traveler away.
Dr. Giwa is an Associate Professor of Emergency Medicine with a special interest in combat medicine/trauma, resuscitative critical care, difficult airway management, health care law, and bioethics.
Image by Alexandros Michailidis / Shutterstock
Click here to see more perspectives on COVID-19 from the Doximity network.
Click here for up-to-date news about COVID-19 on Doximity.