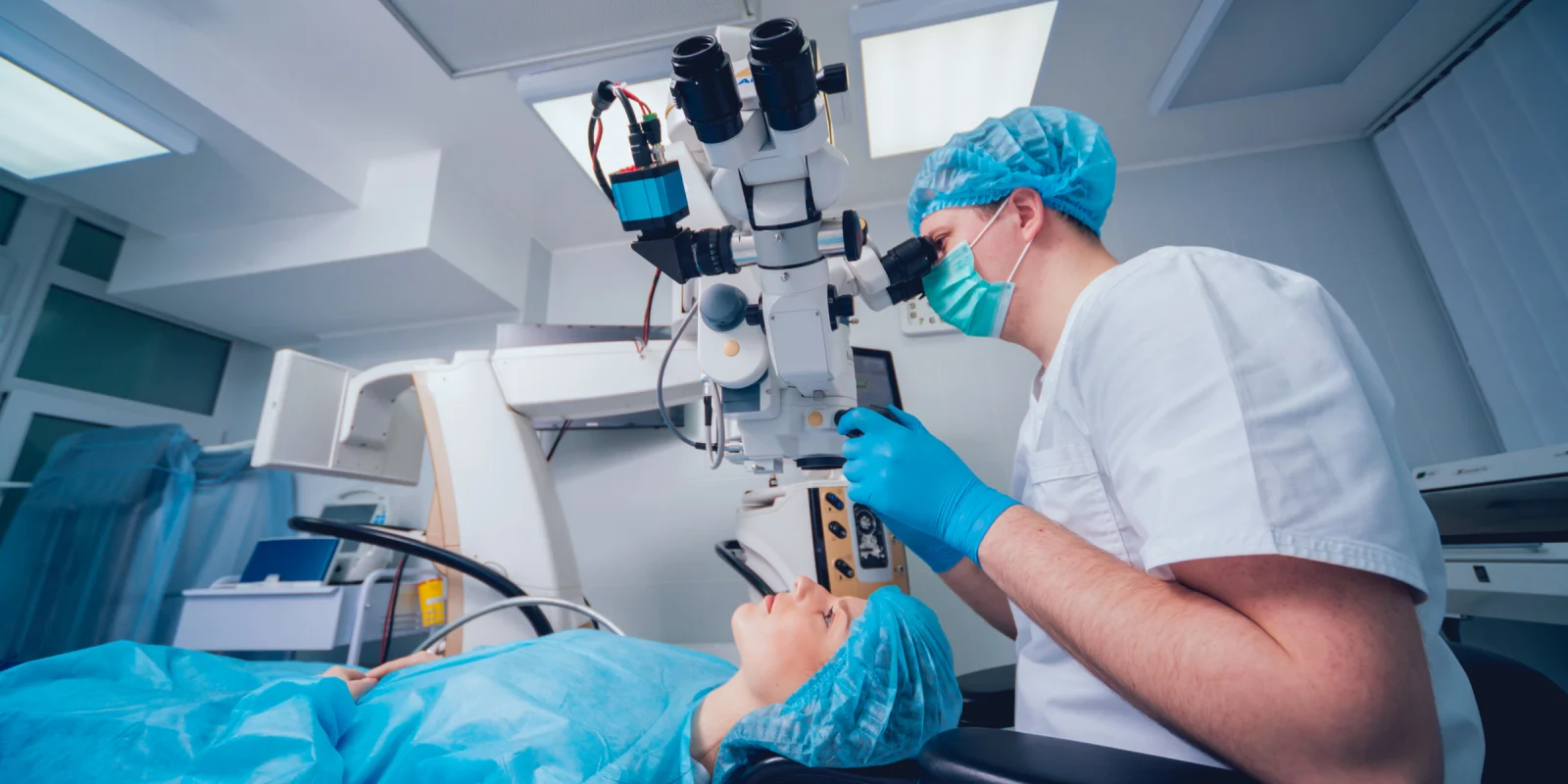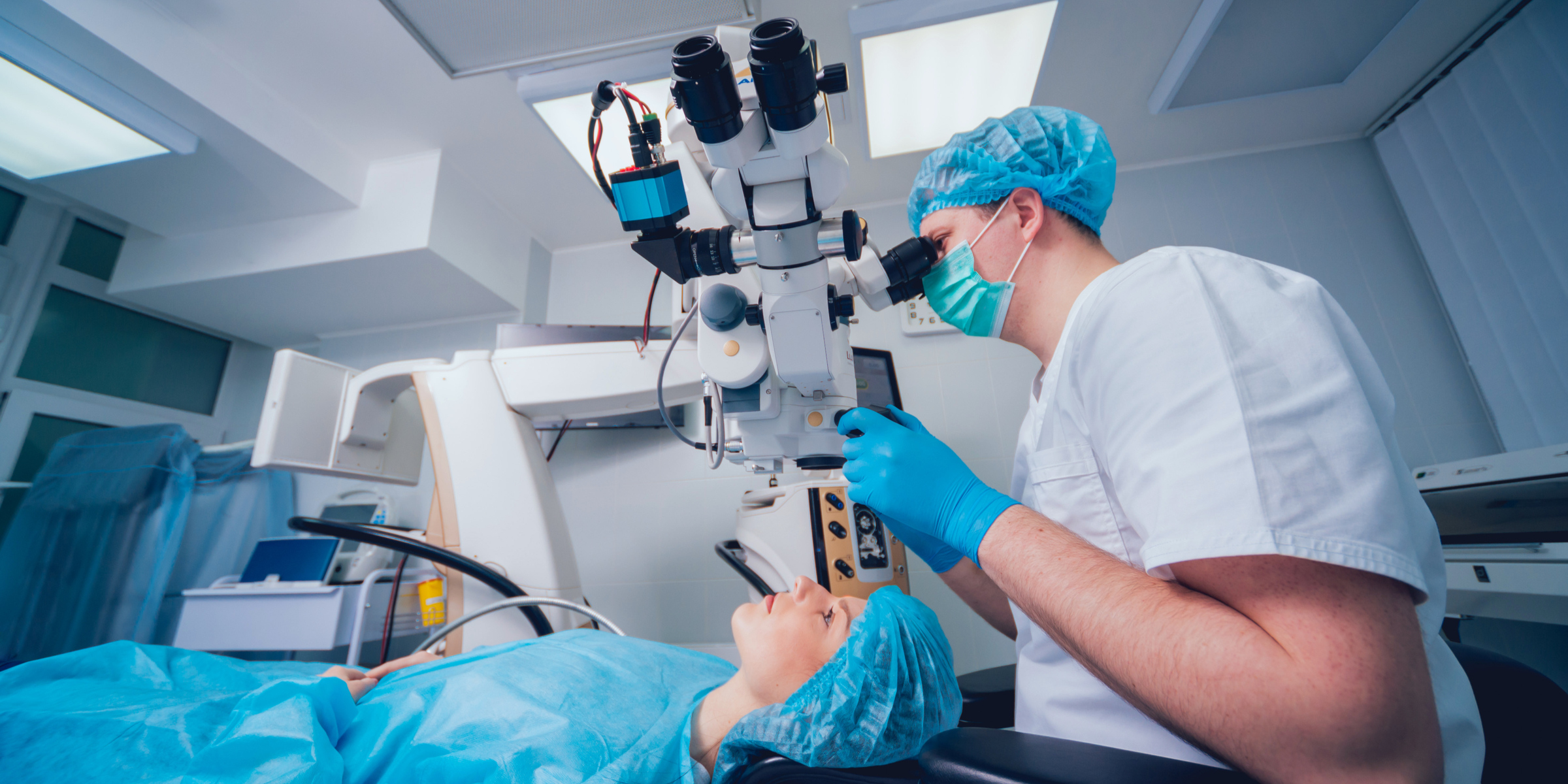
Pre-retinal membrane removal has remained one of the most difficult aspects of vitrectomy surgery, especially when it is performed upon the more delicate fibro-glial membranes of idiopathic macular pucker in an eye following spontaneous vitreous detachment.
The current surgical strategy has been, after removing the vitreous gel, to stain the retinal internal limiting membrane not covered by the overlying fibro-glial membrane, in order to better identify the boundaries and then to strip the membrane(s) from the retina using hand-held, end-gripping forceps, starting at the edge of the pre-retinal membrane in the peripheral macula (in some cases following the initiated uplifting of an edge with a Tano scraper, (e.g.Synergetics) or Finesse loupe (Alcon), and then by peeling toward or around the fovea. Very often this is followed, by the use of the same instruments, applied to the stripping of any remaining internal limiting membrane following re-staining by repeat application of the vital dye (to reduce recurrence of the pucker).
While the patient can appreciate that the distortion is subjectively improved along with some improvement in the measured visual acuity, there often remain post-operative central or paracentral visual field defects (VFDs). These typically are not routinely evaluated post-operatively, either because the surgeon does not measure the central field, or when it is done, it’s of insufficient sensitivity to detect small defects such as when performed with the Humphrey Visual Field 24-2, which fails to adequately examine the macula (Hood) — which requires 10-2, microperimetry, or Omnifield central resolution perimetry — under functional conditions similar to that which occur under natural, low-photopic or mesopic working conditions of everyday tasks (Yavuz, Gutstein).
The question that remains is what causes these post-operative defects and how might they be reduced or avoided? At first, when the staining of the membranes was performed using Indocyanine Green Chorioangiography, a toxic effect of the dye was suspected (Haritoglou), but the defects remain even with the use of other vital stains. Are they due to the less-than-ideal grasping and stripping technique by the surgeon holding the forceps that unwittingly injures the internal retinal layers? When the VFDs in our own experience were overlaid on the post-operative OCT, they corresponded to focal defects in the nerve fiber and ganglion cell layers. When we reviewed the surgical procedure video, the visual field defects did not correspond with the areas where the membrane edge was originally grasped but occurred at various points along the stripping path. When overlaid on the pre-operative OCT, they appeared to correspond to areas of more diffuse ERM adhesion, but not necessarily at points of focal vitreous adhesion or over vessels where one might expect a more tenacious adhesion.
The defects therefore are caused by the traumatic stripping with tools held in the hand in which the surgeon causes inadvertent antero-posterior jerking motions that tear the inner retina rather than atraumatically releasing the membrane(s). At ASRS, the group of Rosen et al, utilizing the Preceyes Surgical System robotic instrument manipulators in animal studies and in human vitrectomy simulations, when compared with the human hand, reduced tremors and jerks from often more than 100um in surgeons’ hands to less than 10 um (Rosen).
In addition, by enabling the surgeon to better visualize the induced traumatic distortion of the inner retina during the stripping, the methodology could be improved. Under current visualization through the microscope, the surgeon’s stereopsis is certainly limited by the effective inter-pupillary distance through the patient’s dilated pupil. However, the stereopsis is also limited by the AP direction of the surgical lighting, which removes the shadows and hence, the visualization of all texture and deformities. Although the suggestion has been made to use an intraocular lighting probe with a prism or angled mirror to provide lighting that is parallel to the retinal surface to better visualize such distortions, this has never been implemented. Rather, the industry has gone in the direction of developing intraoperative OCT. The questions remain, however, whether the OCT visualization in its current form can be provided with sufficient frequency (producing an interactive video) and with minimal latency so that the results can be visualized while the membrane and underlying retina are manipulated. Dr. David Kim presented the effects of video feedback latency on performance (using an interactive simulation) and demonstrated that latencies less than 122 msec. had minimal effect on a simulated peeling procedure with 3D HUD visualization, when the surgeon was sufficiently trained with the involved latency (Kim).
If these developments can be produced and provided, the surgeon could be trained with interactive teaching videos, which should result in significant improvement in outcomes. Additionally, if intra-operative or pre-operative medications were available which would reduce the adhesion (such as ocriplasmin or chondroitinase), this could potentially improve the outcomes and reduce complications.
References:
1. Gutstein W, Sinclair SH, Presti P, North RV (2015) Computer measurement of central visual acuity under mesopic and glare conditions in eyes with nuclear cataract. J Comput Sci Syst Biol 8: 6: 354-366 doi:10.4172/jcsb.1000210
2. Haritoglou, C., Gandorfer, A., Gass, C., Schaumberger, M., Ulbig, M., & Kampik, A. (2003). Effect of Indocyanine-Green on functional outcome of macular pucker surgery. Am J Ophthalmol, 135, 328-337.
3. Hood DC, Raza AS, de Moraes CG, et al. Glaucomatous damage of the macula. Prog Retin Eye Res. 2013;32:1–21
4. Kim, DTT, Chow,DR. The effect of latency on digital vitreoretinal surgery, ASRS paper presentation, 2020. https://meeting2020.asrs.org/presentations#/the-effect-of-latency-on-digital-vitreoretinal-surgery-7270
5. Rosen, RB, Ladha, R, de S, MD. Time independence, optimized surgical steps- The promise of robotics, ASRS paper presentation, 2020 https://www.asrs.org/content/documents/technology_rjuly-10.pdf
6. Yavuz, GA., Unver, Y. Bekiroglu, N. Presti, P., Sinclair., SH (2009). "Central field perimetry of discriminated targets: I. Results for normal individuals using high-contrast targets." Eye 23(11): 2082-2089.
Image: Roman Zaiets / shutterstock