The need for PPE is real. Hospitals across the globe have reported shortages of all kinds of equipment critical to managing COVID-19, from ventilators to respirators to face masks.
Governmental bodies and public health organizations such as the WHO and CDC have acknowledged that the global stockpile of PPE is insufficient and offered strategies for PPE optimization to support front-line workers. Though well-received, these efforts have fallen short of meeting the ever-growing demand for critical supplies, prompting concern among health care executives and clinicians.
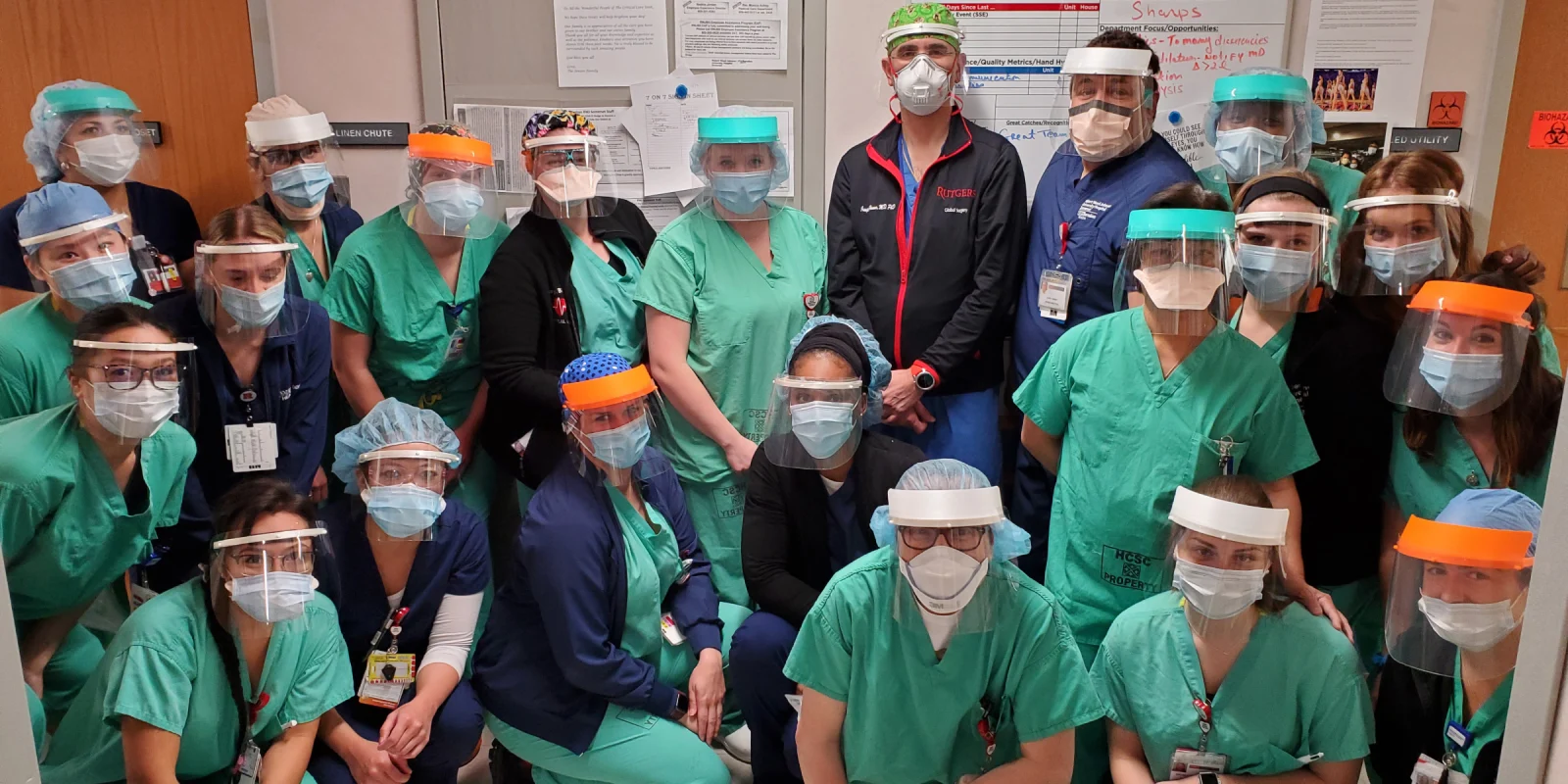
This concern has been no more apparent than at Rutgers Robert Wood Johnson University Hospital, a level one trauma center in New Jersey that has been inundated with COVID-19 cases since the onset of the pandemic. Clinicians at the hospital, including acute care surgeon Joseph Hanna, MD, PhD, regularly come in contact with severely ill or injured patients and are exposed to tremendous transmission risk.
“Along with other PPE, face shields are crucial for those of us taking care of patients, especially during high-risk procedures, where there’s a real possibility of getting sputum or large respiratory droplets in our eyes or face,” Dr. Hanna said. “Yet by the time the pandemic really started to ramp up at our hospital, we noticed that we just didn’t have enough.”
The exponential growth in cases had rapidly gutted the hospital’s resources early on, limiting its ability to provide adequate protection for clinicians. But they continued to fulfill their duties nonetheless. One by one, clinicians started to contract COVID-19, which compelled many to leave their posts for extended periods of time.
As anxiety among health care workers mounted, Dr. Hanna realized that something had to be done, and that he and his colleagues would have to be the ones to assume the mantle. “The PPE shortage across the country is a significant problem, not because hospitals and health systems aren’t trying to source what’s needed; it’s just extremely difficult to get a hold of in sufficient quantities,” he said.
To that end, he partnered with Rutgers University leadership to develop a strategy to independently manufacture PPE. For a 3D printing enthusiast like Dr. Hanna, the solution was immediately obvious: leverage 3D printing.
The FDA in March issued a statement sanctioning judicious use of 3D printing technology to create PPE (and other gear intended to protect a wearer from the spread of infection). Joining the cause, the NIH launched an online portal dedicated to 3D printing PPE designs reviewed in clinical settings.
These initiatives laid the groundwork for Rutgers to manufacture PPE in-house, without having to rely on commercial suppliers. Encouraged by these measures, the university decided to enlist staff from the Department of Biomedical Engineering to use existing 3D printers and laser cutters to produce 3D-printed face shields and intubation boxes, as well as other essential equipment.
Within two weeks, the roughly 30-member team had devised a standardized technique allowing for the production of 500 reusable 3D-printed face shields per week. Their workflow covers the entire process, from 3D printing and assembling individual parts to sanitizing and distributing the face shields. An important quality of these masks is that they are reusable, Dr. Hanna said, “so even though the numbers sound small, it’s actually huge at our hospital.” The team has thus far equipped the hospital’s anesthesia, obstetrics, emergency medicine, and ENT departments with approximately 1,500 3D-printed face shields.
“The good news is that it’s not just us working on this,” he said. “People are engaging at an incredible level to help front-line workers, and the PPE supply is becoming more readily available.”
Indeed, efforts by medical groups and individual physicians are emerging all across the nation:
- Koushik Kasanagottu, MD, an internal medicine resident at Johns Hopkins Bayview Medical Center, is leading a similar effort to make 3D-printed face shields for clinicians in Baltimore.
- Radiologist Beth Ripley, MD, PhD, from VA Puget Sound Health Care System and director of the hospital’s 3D Printing Network, spearheaded an initiative to create 3D-printed face masks. Her group’s latest design meets regulatory standards, capable of protecting wearers from tiny aerosols.
- In the South, anesthesiologist Bryan Lai, MD, and colleagues from the University of Texas Health Science Center at San Antonio have developed a low-cost 3D-printed ventilator circuit splitter that enables clinicians to use a single ventilator for multiple patients.
But how might clinicians or hospitals without access to 3D printing resources replenish their PPE stock?
The best route in such cases may be to look towards the community for support. According to Dr. Hanna, volunteer work from a nearby community college has helped double the engineering team’s PPE output over the past couple of weeks. “What I’m hearing across the Northeast is that hospitals are benefiting greatly from community engagement,” he said.
That was precisely the approach Uyen Caro, MD, embraced when her medical center’s PPE supply ran low. As a hospitalist assigned to the COVID-19 wing at Baton Rouge General Medical Center, Dr. Caro recognized right away the pressing need for PPE. So she turned to her husband, Dane Caro, a programmer and 3D printing expert, and together they brainstormed ways they could contribute.
“Due to the global pandemic, we had to get creative,” she said. “We initially toyed around with the idea of 3D printing N95 respirators but eventually decided the 3D-printed face shield would be the most efficient and cost-effective piece of PPE to produce.”
After settling on a design, they reached out to local business incubator Louisiana Technology Park in hopes of finding a partner to help them manufacture the face shields. Word of their request soon spread throughout the region, drawing interest from numerous community members. Collectively, the group has managed to produce 2,003 face shields, all of which they donated to clinicians in south Louisiana.
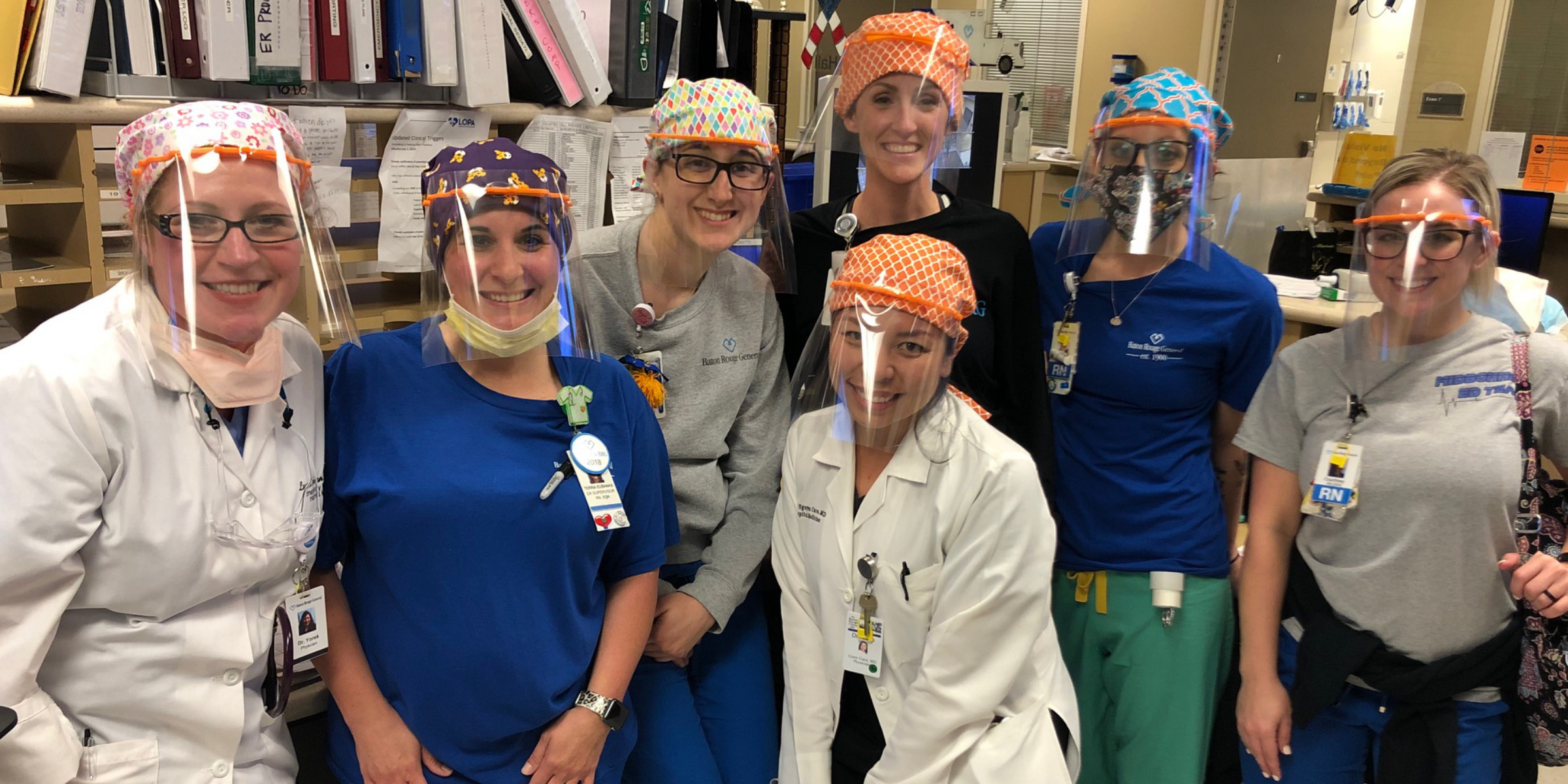
“The outcome showed how loved and supported health care workers are in the community, making our days brighter during this dark and exhausting time,” Dr. Caro said.
Filling the gap in PPE has not only provided necessary protection to medical staff but also contributed to relieving a huge emotional toll for clinicians faced with “surreal levels of critical illness,” Dr. Hanna said. “We don’t want to lose anybody and certainly don’t want to lose colleagues. Because of the amazing efforts of hospitals to secure PPE for clinicians through grassroots movements like ours, we’re not seeing as high of an infection and death rate. And that has been hugely, immensely satisfying.”
How has your hospital addressed PPE shortage amid the pandemic?
Click here to see more perspectives on COVID-19 from the Doximity network.
Click here for up-to-date news about COVID-19 on Doximity.
Photos courtesy of Joseph Hanna, MD, PhD, and Uyen Caro, MD.