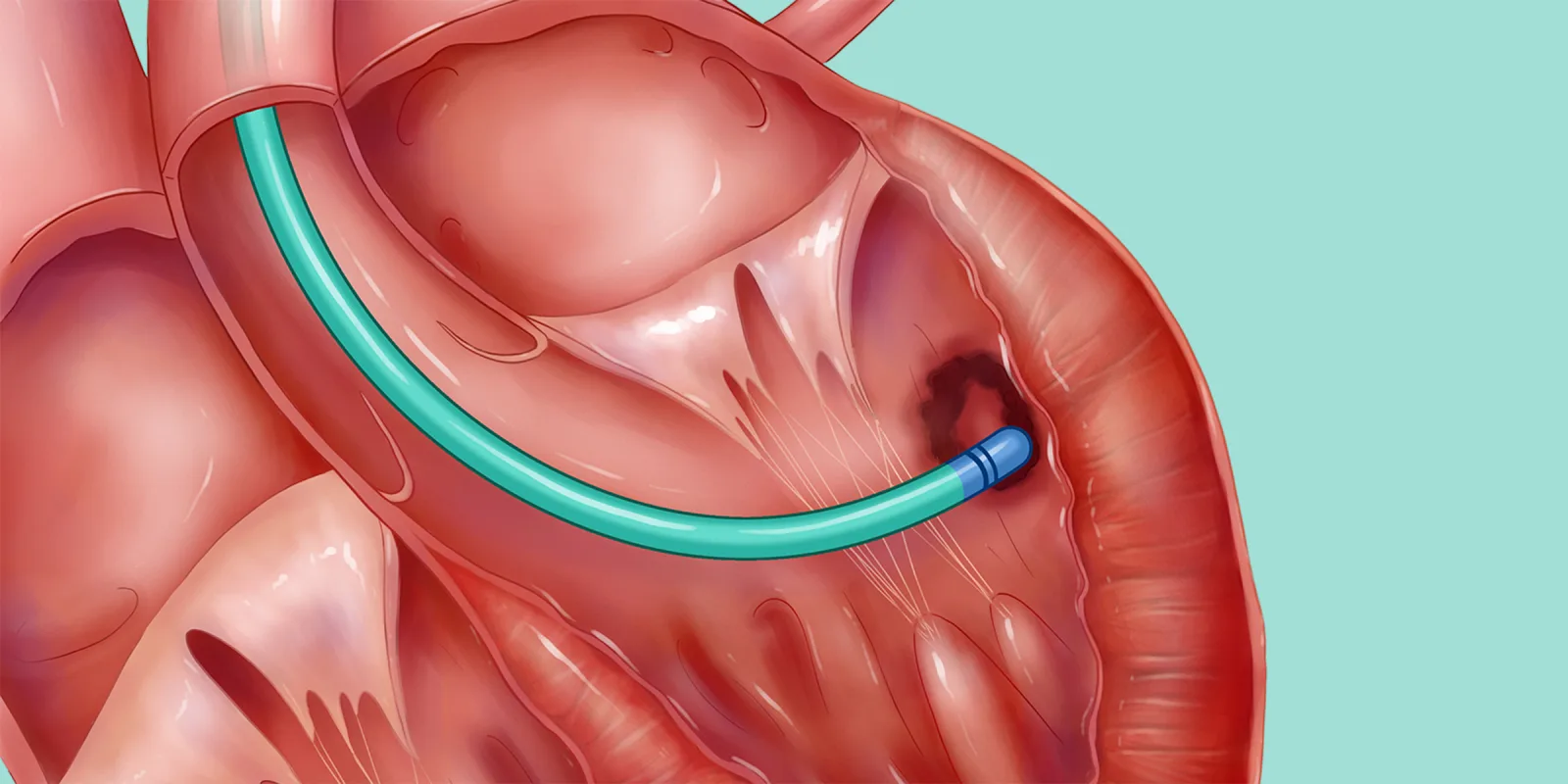
The recent Heart Rhythm Society 2021 offered the attendants numerous interesting studies. From the perspective of an ablationist, I was drawn to the results of the PAUSE-SCD trial. The clinical question was whether prophylactic ventricular tachycardia (VT) ablation before ICD (implantable cardioverter-defibrillator) implant could improve outcomes. Previous studies had focused mainly on the ischemic substrate. That is, ventricular tachycardia originating from exit sites in chronically injured or infarcted myocardium.
To put things in perspective, suppression of VT can be difficult with the available antiarrhythmic therapy. Notably, this broad class of Medications is associated with significant adverse effect profiles. VT ablation is often performed In a palliative manner when these agents do not effectively suppress arrhythmia. Patients who present with ventricular tachycardia are invariably considered for ICD implant. Notwithstanding, these patients have device programming schemes to attempt painless pace termination. This may be effective perhaps half the time, often requiring a defibrillator shock to terminate VT with the remaining episodes. All patients who have experienced such a shock will categorically indicate that this is a very painful experience. Some patients develop posttraumatic stress because of this. Additionally, shocks may ultimately compromise patient longevity. A method or technique which could lessen the burden of VT would be desirable.
In 2007, Reddy et al. published results from the SMASH-VT trial, which randomized patients to a prophylactic substrate-based ablation before ICD versus ICD implant alone. Although this was a small study (N=128), the results were in favor of empiric ablation to reduce the incidence of ventricular tachycardia events, but not mortality. Significant complications were few. Three years later, Kuck and colleagues shared results from the VTACH trial, similar in design and study population. This trial was also a small randomized study (N=107) which concluded that prophylactic VT ablation did appear to reduce future VT events. More significant complications were, however, observed. Both of these studies were too small to adequately evaluate mortality. Nevertheless, when taking both of these studies into context, one could surmise that there is a role in selecting patients who present with monomorphic ventricular tachycardia to be considered for a prophylactic ablation before an ICD implant. What is unclear from both of these papers is how critically sick some of these patients were. Ablation for ventricular tachycardia can be associated with complications.
The data presented by Tung also suggested a benefit with early ablation after VT presentation before ICD implant. This multicenter study was comparable in size (N=121) to SMASH-VT and VTACH but was unique in that all etiologies of VT were included. Moreover, patients were enrolled from sites in Asia. Freedom from VT was more often observed than in the control group who received an ICD without intervention. The study population did have a minority of serious procedural complications as well. The results of this study indeed reinforce the answer to the question of whether a prophylactic ablation for substrate VT may reduce the risk of recurrence. However, we must be clear that this type of ablation is invariably palliative given the fact that the recurrence or appearance of new VTs was observed In all three of these studies. Additional
work is needed to enhance the efficacy of VT ablation, perhaps guided by MRI or not all imaging strategies.
Dr. Christian Perzanowski is employed by Bay Area Cardiology. He has no conflicts of interest to report.
Illustration by Wendy Gu