Early this year, I took two months away from my private practice and traveled to Haiti and Vietnam to teach surgical and clinical skills to physicians, working with Health Volunteers Overseas. This was not my first medical mission trip, as I have been leading surgical teams to Haiti every year since 2006. However, by providing a “fly-in” package, I realized that we were contributing more to the long-term problem of developing world medical care than we were helping. Haitian physicians were so busy taking care of the day-to-day needs of their patients that they seldom had time to participate in learning new skills when our surgical team arrived. The Haitian patients saw the doctors from the United States as better doctors because they did the more complicated surgeries. Instead of working ourselves out of a job, which should be the aim of medical missions, we were making the problem even worse.
Health Volunteers Overseas provides physicians and other health care providers with a different option. They coordinate with hospitals throughout the world to improve the availability and quality of health care through the education, training, and professional development of the health workforce. Less doing and more teaching, in the hope that improved health care can be provided by an in-country workforce that has both the cultural background to understand patient care and the skills to provide the health care that is needed.
In the months prior to my departure I spent hours preparing PowerPoint presentations, downloading surgical videos, and collecting teaching tools. Once I arrived, I spent the first few days simply listening, only offering input if I was asked. Even with an interpreter, it is often difficult to understand a hospital system that faces dramatically different challenges than we do in the U.S. And then came the difficult part. I tried to unteach some bad habits and re-teach with new information. Change is difficult for everyone, but I think especially for physicians. We have spent so much of our early adult life in school — we don’t want to think that some of what we learned may have become outdated or simply false.
Due to language barriers, much of the recent medical information that is available from the developed world is not accessible to those in health resource-poor countries. These same countries often have access to newer technologies but lack experience in the scientific know-how of interpretation. Access to, but lack of education surrounding, ultrasounds is a good example. I spent many afternoons discussing the difference between benign and abnormal findings in the female pelvis, as well as how best to explain to patients that surgery was not always in the patient’s best interest.
No matter how much time I have spent in overseas hospitals, I am reminded that I am both the student and the teacher. In Haiti, I am always amazed at the prevalence of chronic hypertension and severe preeclampsia in pregnancy. A busy maternity ward often has 3-4 women in the early third trimester with blood pressures of 150-160/90-100. In the U.S., we would treat them with steroids for 48 hours to improve fetal lung maturity and then get them delivered. We have the advantage of an excellent neonatal intensive care unit with survival rates of 95 percent beyond 28 weeks. The lower limit of viability in most Haitian hospitals is 34 weeks. It is the norm to keep these severely ill women pregnant well beyond what we would consider advisable in our country. Haitian physicians seem to understand when they have pushed the envelope far enough in gestation and the benefit is in delivery and not in pregnancy.
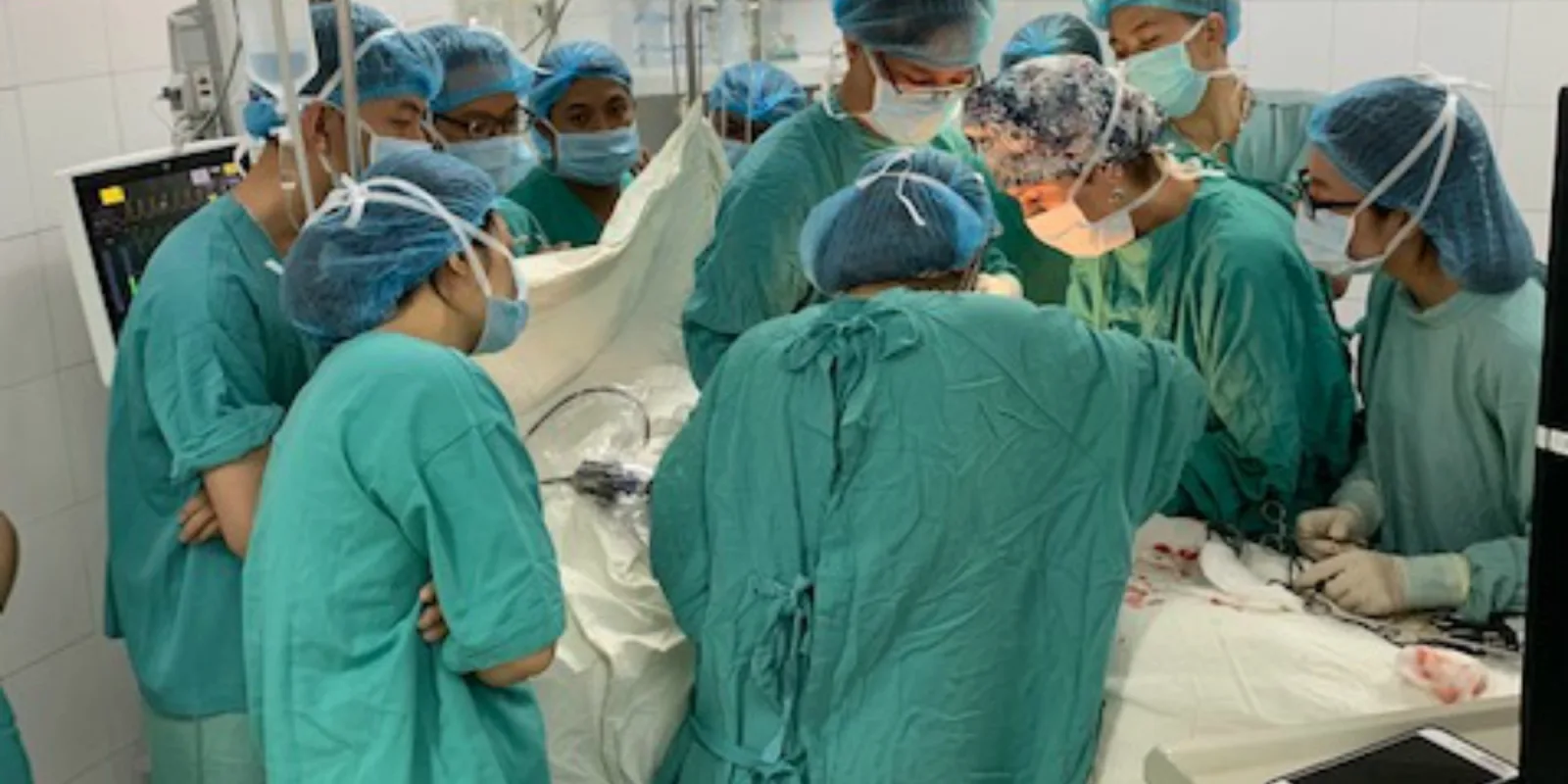
As another example, I’ve noticed that resource-poor countries have never become enamored with the disposable waste system that is associated with western medicine. This is not only due to cost but also to the lack of a medical waste incineration process. Gowns and operating room drapes are cloth; they are re-washed and sterilized after each use. Disposable instruments are not to be found. Bovies are cleaned in cidex and reused. The skill of a surgeon is often gauged by how many times s/he can re-use the same suture. The lack of an appropriate reusable product challenges these physicians to create their own substitutes. I witnessed a Vietnamese surgeon create a surgical retrieval bag out of a large piece of sterile plastic, purse-stringing a piece of suture around the top edge, accordion folding it to fit through the port, and then carefully opening inside the patient to retrieve a large ovarian cyst.
The physicians from these countries should be in charge of what is “taught.” What we as outsiders think is helpful may result in untoward consequences because of cultural misunderstandings. After all, we are only in the country for a short time. An experienced provider needs to be available to deal with both short- and long-term complications. There are still circumstances where fly-in trips to provide medical care may be helpful — but they should be the exception and not the rule. Empowering indigenous health care providers should be the primary aim of most medical mission trips.
Dr. Leslee Jaeger is an Ob/Gyn and a 2018–2019 Doximity Author. She is also a mom to three biological and two adopted children, an advocate for women’s health domestically and internationally, and she loves good food and good books. Dr. Jaeger writes about her family and work on her blog.